Bedside robots and AI for triage – this is the future of the NHS if it wants to survive
We should not accept an analogue NHS in a digital decade
The extra £20bn a year secured by Jeremy Hunt as a 70th birthday present for the NHS is a very large sum. It will never be enough, of course, and doomsayers are claiming the money is already spent – on unfunded deficits, pay deals and a maintenance backlog. But most senior NHS figures agree that no secretary of state could have extracted more from the chancellor.
The priority now is to see that the money is spent wisely. History shows that it is developments in science and technology – and not the multiple NHS re-disorganisations – that have had the biggest impact in transforming care, from hip replacements to heart transplants, magnetic resonance imaging (MRI) to effective drug treatment for HIV/Aids.
Innovation is the key to the NHS’s future. Without innovation it cannot survive. Genome sequencing, 3D printing, immunotherapy, artificial intelligence – all hold huge promise. They offer the prospect of better care delivered more efficiently, producing more bang for every buck.
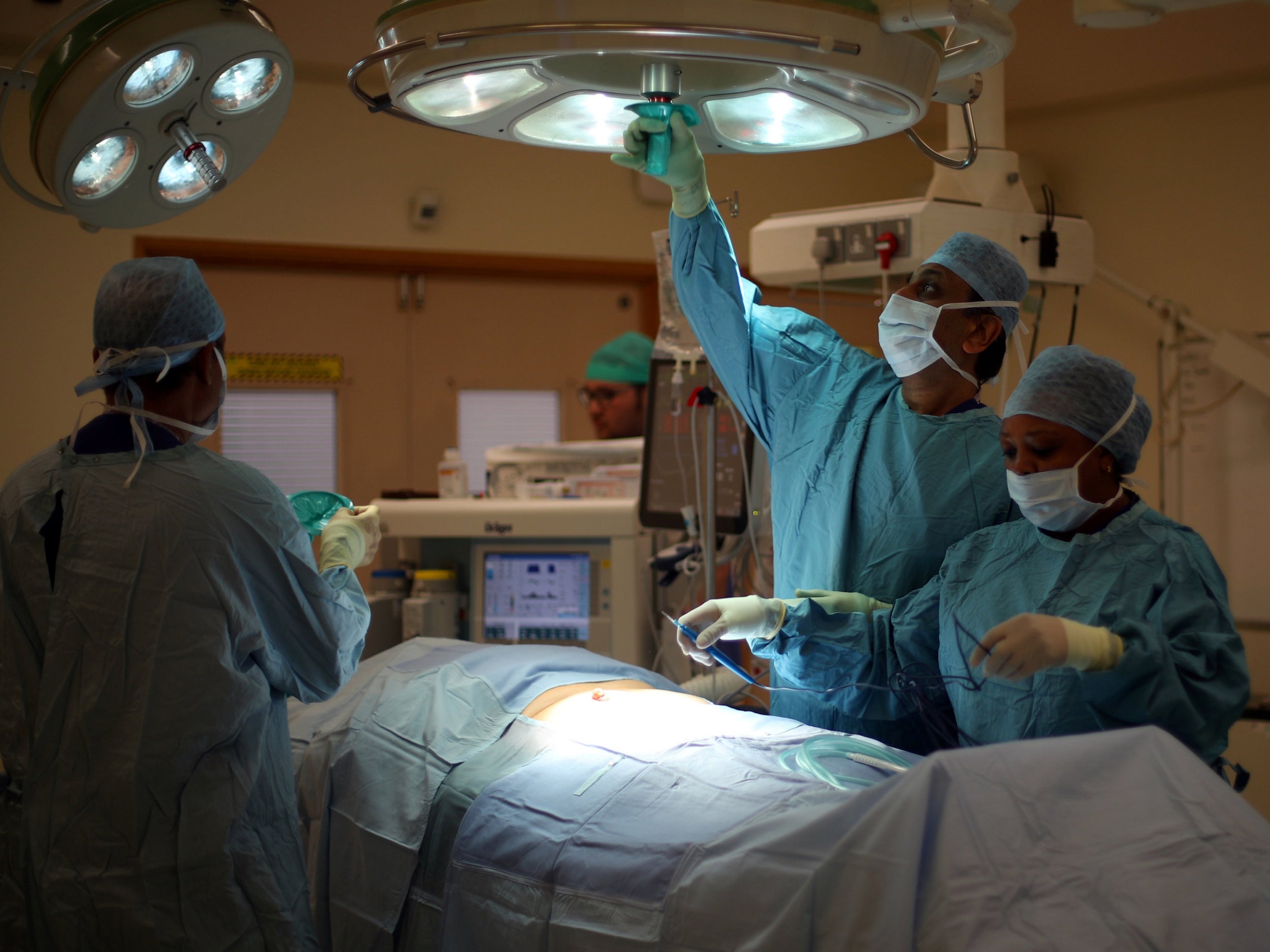
17 years ago I performed the first operation in the UK using a surgical robot. As it happens, that is the average time it takes for an innovation to spread around the NHS. And today, updated versions are widely available, giving surgeons a magnified view of the operative field and allowing them to cut and stitch with great precision, reducing errors, improving care and speeding recovery.
But 17 years? It is far too slow. That is why a new joint government-industry group, the Accelerated Access Collaborative, which I chair, will shortly be launched to identify the most transformative medical innovations and ensure they are available on the NHS up to four years earlier than at present.
Surgical robots have an undeniable glamour – science fiction made science fact. Tomorrow’s advances are likely to come from a more humdrum source: those dog-eared notes that used to fill every GP surgery and hospital records department.
Now largely digitised, the NHS’s store of 60 million medical records represents a unique data repository that is both vital for individual treatment and an unmatched source of insight for researchers. With the help of artificial intelligence and machine learning to mine these vast datasets, we have the chance to change the model of care from “diagnose and treat” to “predict and prevent”.
New technologies are changing the way care is delivered and how it is provided. People spend hours on their smartphones daily, but typically see a doctor or health professional just once a year. Mobile apps to help patients track changes in their health and respond appropriately are bringing quicker treatment and lower costs.
These are among the benefits now within our grasp; the challenge is how to unlock them. While tech is transforming society, it has yet to do so in the NHS. We are among the last users of fax machines, the last to communicate by letter, and it is a scandal that patients still arrive in A&E without doctors knowing what medicines have been prescribed, because of restrictions on data sharing.

In my Review of Health and Care, published in June by the Institute for Public Policy Research, I set out a radical plan to streamline the NHS and make social care free to ensure the health and care system is fit for the 21st century. A key part of the plan is a “tilt to tech” to achieve a digital first health and care system.
Underinvestment, lack of interoperability (systems that don’t talk to one another) and problems with security highlighted by the WannaCry ransomware attack which disabled hospitals and GP surgeries across the country in May 2017, have hindered progress. But the potential benefits are huge.
By embracing full automation of administrative and repetitive tasks – while offering all staff affected the right to retrain – we estimate the NHS could save £12.5bn a year (and £6.5bn in social care) and free staff to focus on treatment and caring.
From fully automated assessment. or “triage”, of patients attending A&E to bedside robots assisting with meals, transport and mobility, from biosensors allowing remote monitoring of patients at home to systems that alert clinical staff when a hospital patient’s condition is deteriorating, there are enormous gains in prospect. But only if we have the courage to seize the opportunities.
When the NHS was founded, we led the world by example. As the NHS celebrates its 70th birthday, we have the opportunity to lead the world once more. We should not accept an analogue NHS in a digital decade.
The health and social care system needs a comprehensive strategy to harness 21st century technology and innovation at pace. This should be among the biggest priorities for politicians and policymakers today.
Professor the Lord Darzi of Denham, OM, is Paul Hamlyn Chair of Surgery at Imperial College and a surgeon working in the NHS. He was parliamentary undersecretary of state for health from 2007 to 2009
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks