Unless we fight for the future of the NHS, we risk returning to a wealth-before-health service
Without the resources needed to tackle the waiting list backlog, we will have a health service that resembles that of the first half of the 20th century

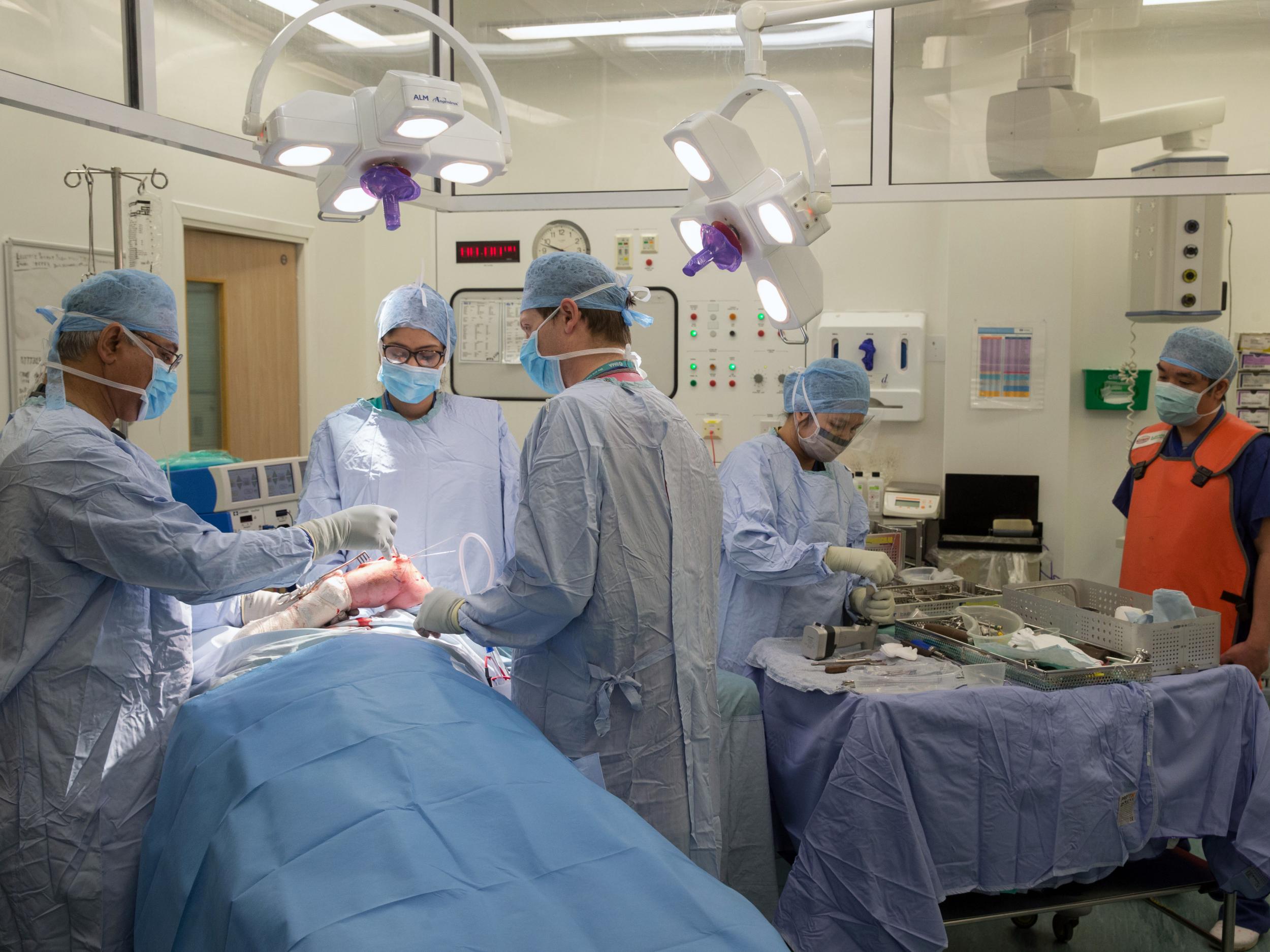
“No society can legitimately call itself civilised if a sick person is denied medical aid because of lack of means,” said Aneurin Bevan. As a doctor, the above reflection from the NHS’s founding father has been weighing heavy on my mind this summer.
With the government busy negotiating the balance between restriction and infection, pressure levels for NHS services and waiting times for many patients have crept higher and higher. At the end of May, over 300,000 patients had been waiting more than a year for treatment following a consultant referral. These are full years of people’s lives that may be spent in pain or fear, with many unable to carry out normal activities or their conditions getting worse.
A Commonwealth Fund report, released this month, downgraded the UK from first to fourth place in their ranking of national healthcare systems, in part because of the increased average length of waiting times.
However, those who can afford it can jump the queue and seek private treatment. Sometimes this even means getting the same surgeon who would have eventually treated them in the NHS.
But with the price of blood tests and scans running into hundreds of pounds, and major operations such as hip replacements costing several thousands, this is a solution only available to an elite group. Those who do not have the money for private treatment are left behind. With almost twice as many lower income Brits claiming to have experienced cost-related barriers to care over the past year (compared to those in the higher income bracket), a new type of health inequality in the UK is growing.
Unless we give our overstretched NHS the resources it needs to tackle the waiting list backlog, we are likely to find ourselves back somewhere that looks remarkably like the first half of the 20th century – a time before access to free healthcare at the point of use was fervently embraced across Britain.
The health and social care system in England risks developing similarities with its bottom-ranked American counterpart, where exorbitant costs regularly bar the low-income and the uninsured from accessing treatment. Whilst the similarity stops there, the trend is worrying. However, it’s not too late to reverse this escalating crisis if we push for a coordinated, properly resourced effort to deliver sustainable change.
We need to focus on the reasons why over 5 million patients – a number that could soon rise to 13 million – are languishing on waiting lists. Whilst Covid-19 has played a huge role in this, it is by no means the primary cause - which is why time won’t heal the problem. As a surgeon, I know how hard NHS teams work to balance the huge numbers of patients needing planned care with those requiring emergency interventions. But to succeed, their efforts must be underpinned by a number of essential, organisation-wide transformations.
Firstly, we need to make sure that we have enough boots on the ground. From nurse practitioners to night porters, staff are the lifeblood of the NHS. But currently they are burning out and exiting at unprecedented rates, pushed to the brink by inflexible rotas, exhausting high-pressure shifts and inadequate pay rises. Staff shortages mean more cancelled care and even longer waiting lists; it follows that investment in training as well as retention initiatives, wellbeing campaigns, mental health support, and tech that supports smarter dialogue and support and flexible working, must be fast-tracked. The government must ensure NHS trusts have the resources to bring in new staff whilst ensuring the existing and future workforce can be retained.
Secondly, we need to take a long, hard look at how to modernise and connect the clunky systems that staff have to struggle with on a daily basis. Too much clinical time is wasted, and too much valuable information made inaccessible, by years-old software and tools not fit for practice. Newer, more powerful and efficient options are available - the NHS needs to embrace them if it wants to maximise the capacity of its current staff and make it easier for them to do their jobs.
To really make a dent in waiting times, we also need to find sustainable ways to redistribute the pressures on hospital services and overwhelmed GPs, as well as respond to emerging pressures such as the escalating mental health crisis. This demands a tightening-up of how we triage patients, a strengthening of primary care’s ability to offer patients a range of care avenues, and a strategy to reduce the number of unnecessary referrals eating up consultant time. This, however, won’t be possible until the different parts of the NHS secure the means to communicate and collaborate effectively, then have the funding needed to capitalise on it.
In our digital age, when surgeons can perform complex operations from thousands of miles away, it’s unacceptable that a lack of technology is preventing GPs, paramedics and community health workers from working in partnership with hospital consultants, emergency department managers and patient transport services. Patients are slipping through nets time and time again, GPs are wasting hours chasing up the latest guidance or manually updating patient records. It’s no wonder that 1 in 5 NHS staff are planning on changing careers once the pandemic is over.
There are no shortcuts when it comes to tackling the waiting list mountain, but it’s vital we use every existing and prospective tool in our arsenal to chip away at its bulk as quickly as possible.
Aneurin Bevan also once said: “It [the NHS] will last as long as there are folk left with the faith to fight for it.”
If the past year and a half has taught us anything, it’s that we have the deepest and most loyal faith in our national health service; now is very much the time to fight for it.
Dr Owain Rhys Hughes is a surgeon and CEO of Cinapsis
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks