Why patients must rely less on doctors: Improving our own health is the 'blockbuster drug of the century'
Unless people become more involved in their own care, says Jeremy Laurance, health services such as the NHS will collapse beneath the expectations of growing and ageing populations
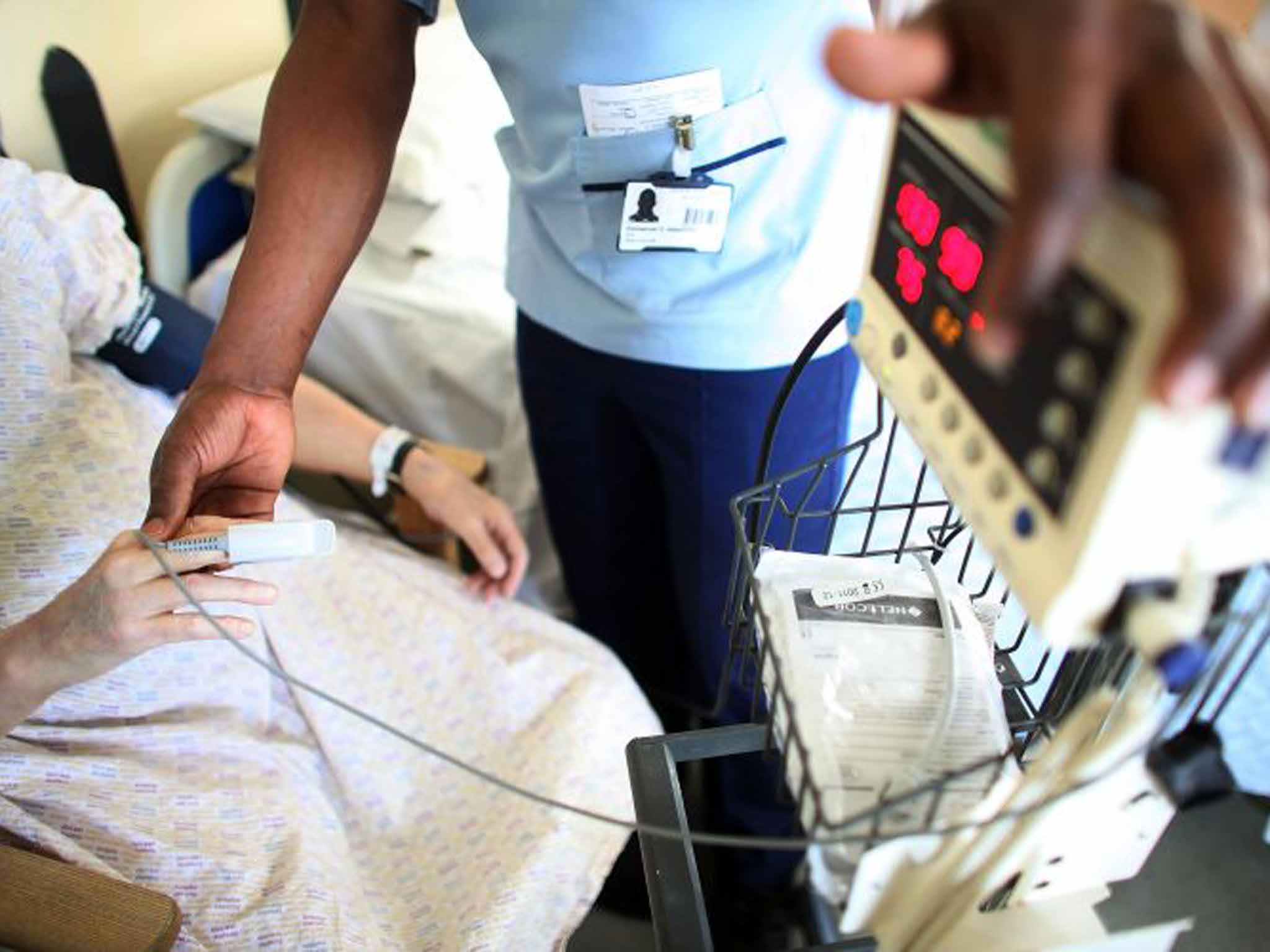
Virtually all of us are or will be patients at some point in our lives. It is strange, then, that when you think of the immense effort, time and resources invested in the NHS, the most important experts – ordinary people managing their own health – are typically left out of the equation.
But perhaps it is not so surprising. Why would doctors and nurses want to help people look after themselves? It is tantamount to a top restaurant learning that their new task is going to be – in addition to serving splendid food in a smart environment – teaching people to cook at home. Why undermine the business by running cookery classes?
The fact is that health costs are rising faster than our ability to meet them – not only in the UK but across the world. The answer to the crisis is not going to come from doing more of the same. Instead, we must harness the energy of patients and the public who care about improving their own health – a huge untapped resource. It has been dubbed the "blockbuster drug of the century".
Leonard Kish, a US health technology expert, who first used the phrase (and the restaurant comparison), gives an example of why patient engagement has such potential. Probably the biggest blockbuster drugs of all time are statins, which lower cholesterol and prevent heart attacks. Millions are taking them. But though they are very good at lowering cholesterol they are less good at preventing heart attacks – only about one in every 99 people on the drugs is helped.
Now compare that with the co-ordinated care programme for patients who have had a heart attack run by Kaiser Permanante, a leading US health insurer. By using technology to engage patients and help them monitor their condition, the overall death rate among patients on the programme was cut by 76 per cent.
If statins are a blockbuster, what does that make patient engagement? Simon Stevens described it in his first major speech as chief executive of the NHS last year as "the coming revolution." Making it happen is a challenge, however.

"Professionals need to get off their pedestals and patients need to get off their knees," says Robert Johnstone of the International Alliance of Patient Organisations. The aim is to change the clinical paradigm from "What is the matter?" to "What matters to you?"
It is helped by the growth of electronic communication, the internet and social media, through which patients are increasingly making their voices heard. From mental health to end-of-life care, sharing experience has proved a powerful tool for raising quality and reducing costs.
Evidence shows that, when patients share in making clinical decisions and are encouraged to manage their own conditions and look after themselves, not only does their health improve but they also make less use of health services.
Shirley Silvers used to be a regular visitor at her GP's surgery in Stoke-on-Trent, usually as an emergency. Aged 66, she has breathing problems owing to Chronic Obstructive Airways Disease, and whenever she developed a chest infection – which was often – she had to make the journey to the surgery to get a prescription for antibiotics and steroids.
Now, with her mobile phone and a few items of basic equipment – thermometer, scales, blood pressure monitor and pulse oximeter (a thimble-like device clipped to the end of the finger to measure the oxygen level in the blood) – she can monitor her condition from her own front room without having to struggle to the surgery to see her GP.
As she can get instant responses from the system – called Florence (after Florence Nightingale) – texted to her mobile, she can act quickly by increasing her medication to prevent her condition deteriorating, thus avoiding an emergency hospital admission.
Shirley is part of the digital revolution that is moving care beyond the hospital and surgery walls into patients' homes.
She says: "I live on my own and I have no one to call if I am in trouble. This acts like a third eye – it gives me confidence. It can be exhausting going to the surgery – but this saves their time and mine. It alerts me to problems before they happen. I have not seen a doctor for more than two years. I think it is amazing."
Flo – as the system is known – has helped Shirley become her own doctor. She has become so adept at using it that she no longer has to rely on texts from the surgery telling her what to do; she measures her oxygen level each morning and manages her condition herself.
Innovative ideas such as this are emerging across the NHS and herald a transformation in care.
They include a digital service for people with mental health problems called Big White Wall, which has more than 20,000 members who share experiences, obtain support and advice and can get one-to-one online therapy from professionals. One-in-four adults will experience some kind of mental health problem in the course of a year and conventional approaches cannot meet this overwhelming demand. The service has reduced GP visits and saved costs and 95 per cent of users report feeling better.
Sue Hawkins, 55, of Alton, Hampshire, whose son Edward was severely injured in 2010 while serving with the Royal Marines in Afghanistan, says Big White Wall came to her aid at a crucial moment after Ed was discharged from hospital.
"He came home for a month. I had to dress his wounds and administer his drugs every day with no support whatever. I went rapidly downhill and became suicidal. I was in a deep dark pit."
She had heard about Big White Wall, found it on the web and registered. She posted her story – itself a cathartic act – and quickly received responses from half a dozen other mothers of wounded soldiers who, like her, complained of the lack of support. "Being heard and being understood – that was really important. I was on Big White Wall for almost a year. It got me back on my feet," she says.

Similarly, patients with dementia are a rapidly expanding group whose care is often poor. Now they or their families can record their choices, medication and care plan on a website called Health Fabric, which ensures that they get personalised care, reducing the use of anti-psychotic drugs and admissions to care home or hospital.
In one Stafford GP's practice of 8,500 patients, the system is estimated to be saving £450,000 annually and it is now being rolled out to 41 other practices in the Midlands.
An online patient-controlled medical records system – operated like a secure version of Facebook – allows patients to share their medical details with all those involved in their care, obtain results of tests, and communicate with their carers directly.
Called Patients Know Best, the system is already used in 30 hospitals and has improved responsiveness, reduced hospital admissions and proved popular with users.
As people increasingly organise their lives on smartphones, the NHS has to change to keep pace. But as the above examples illustrate, the digital revolution also offers an opportunity: to provide care in different ways from the past; more responsive and more personalised while also saving time and money.
Women are a key target because of their pivotal role in preserving the health of their families. In the UK, men typically neglect their health until prompted to attend to it by their partners. Elsewhere, half the global reduction in child deaths over the past 40 years is attributable to the improved education of women, according to a recent study.
An 11-country survey in Australia, Europe and North America in 2011 found that patients engaged in their care reported higher quality, fewer errors and more positive views of the health system. Yet medical staff often fail to recognise the benefits of understanding a person's experience of illness.
The World Health Organisation found such resistance from health workers was common. They needed to be convinced that engaging patients improved the quality of care.
Critics claim that professionals lack the training necessary to be effective team members and the communication skills necessary for establishing partnerships with patients and the public. Professionals complain they do not have time for these important conversations and that it is difficult to fit them into the traditional clinical workflow. But they also deliberately discourage patient involvement by refusing to give people information about their own clinical results, their conditions and other important factors that would improve their ability to manage their own health issues and the coordination of their care.
But while this will be tackled in the NHS under plans to give all patients access to their GP records by 2018 – currently, just four per cent of patients have access – patients and families still face other challenges. Being sick can impair their ability to comprehend or remember information. Even a small problem may create anxiety and fear. The use of medical jargon may interfere with understanding as may a lack of social support.
For those who speak up, fear of retribution or being labelled as a difficult patient may also inhibit engagement.
Individuals also vary greatly in their desire for engagement, ranging from a full partnership to complete deference. Their preferences may also change over time and depend on the burden of illness and the complexity of their condition. The engagement must also be sincere and meaningful on both sides. As one patient on a hospital advisory board remarked: "We want to do more than just have lunch."

There are many levels of patient engagement. It may be a personal event, such as a shared decision between an individual patient and a healthcare professional. It may be a public event, such as a health literacy campaign. It may involve patients and doctors working together to redesign services, improve a hospital's performance or develop self-management programmes for chronic disease.
Whatever form it takes, engagement changes the focus from taking action to improve the health and care of the people, to taking action with the people.
A simple yet radical notion.
In 2009, the 600-bed Beth Israel Deaconess Medical Center (BIDMC) in Boston, Massachusetts, began a drive to increase the involvement of patients and family members in improving care. The hospital appointed 100 patient/family advisers over three years to participate in focus groups, early design efforts and projects across the institution.
These have included improving patient flow in the Spine Centre, planning a new cancer centre and designing a "time out" space for families in the Intensive Care Unit (which has internet access as well as relaxation areas to allow them to get on with their lives). Patient/family advisers sit on 10 committees.
Patients can see test results, communicate with their doctor or practice by email and request appointments and prescriptions electronically. They can check their drugs, allergies and test results for accuracy and many patients have corrected mistakes that could have resulted in medical errors.
A study of almost 12,000 patients given access to their notes at three hospitals, including the BIDMC, found over three-quarters reported feeling more in control of their care and well over half said it increased adherence to their medication.
The message is that patient, family and community involvement may improve the effectiveness of existing programmes as well as extending their reach by giving top priority to the patient experience, an aspect of care too often overlooked. At the same time it may reduce costs and avoid wasting resources on well-intentioned but poorly designed initiatives that are destined to fail.
At the Brigham and Women's Hospital – again, in Boston – nurses in the Intensive Care Unit start their shifts by asking patients: "What is the most important thing I can do for you today?" The answer might be four hours' sleep or a shampoo. A hair wash in the context of medical care costing thousands of dollars a day might seem trivial. But as Kathleen Leone, head of nursing in the unit, points out, it can make the patient feel "like a million bucks".
Even a small gain for individual patients, when multiplied hundreds of millions of times, would translate into a big advance. Engaging patients in their care is not just about saving costs – it is also about helping them feel better.
For the NHS, searching for better ways of delivering care in the face of rising demand and tighter budgets, it could mean the difference between the continued endurance of our most treasured institution and its collapse.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments