Diabetes: Conversion of skin cells to produce insulin could lead to new treatments
Scientists were able to reprogram skin cells before devloping them into the specialised 'beta' cells of the pancreas
Your support helps us to tell the story
From reproductive rights to climate change to Big Tech, The Independent is on the ground when the story is developing. Whether it's investigating the financials of Elon Musk's pro-Trump PAC or producing our latest documentary, 'The A Word', which shines a light on the American women fighting for reproductive rights, we know how important it is to parse out the facts from the messaging.
At such a critical moment in US history, we need reporters on the ground. Your donation allows us to keep sending journalists to speak to both sides of the story.
The Independent is trusted by Americans across the entire political spectrum. And unlike many other quality news outlets, we choose not to lock Americans out of our reporting and analysis with paywalls. We believe quality journalism should be available to everyone, paid for by those who can afford it.
Your support makes all the difference.Scientists have converted human skin cells into the insulin-producing cells of the pancreas. The development could lead to new treatments for patients with diabetes using tissue transplants derived from their own skin cells, the researchers said.
The skin cells were reprogrammed in a laboratory to an embryonic-like state before being grown in a culture medium to develop into the specialised “beta” cells of the pancreas, which manufacture insulin.
Tests on laboratory mice showed that the converted skin cells were able to protect the animals against diabetes, according to a study by researchers at the Gladstone Institutes in the US and the University of California, San Francisco.
“Our results demonstrate for the first time that human adult skin cells can be used to efficiently and rapidly generate functional pancreatic cells that behave similar to human beta cells,” said Matthias Hebrok, director of the diabetes centre at UCSF and a co-senior author on the study published in the journal Nature Communications.
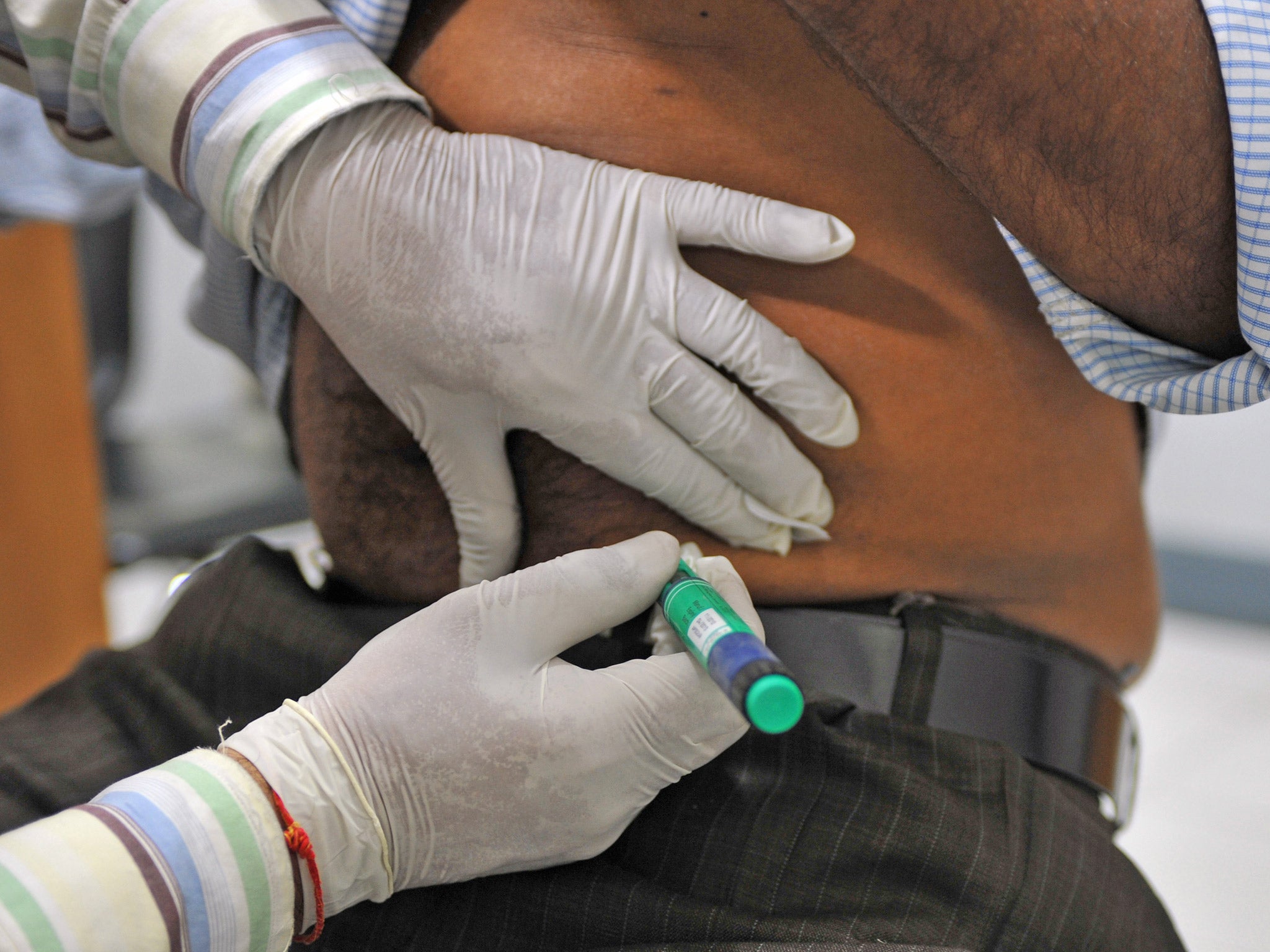
Patients with type-1 diabetes suffer from under-production of insulin and have to compensate with regular injections of the hormone, which cannot be taken in oral form. Developing a way of “repopulating” the pancreas with functioning beta cells would result in an effective cure for the disorder.
“This study represents the first successful creation of human insulin-producing pancreatic beta cells using a direct cellular reprogramming method,” said Saiyong Zhu, a postdoctoral researcher at the Gladstone Institute of Cardiovascular Disease and first author of the study.
“The final step was the most unique – and the most difficult – as molecules had not previously been identified that could take reprogrammed cells the final step to functional pancreatic cells in a dish,” Dr Zhu said.
Sheng Ding, a senior investigator at the Gladstone, and co-senior author on the study, said: “This development ensures much greater regulation in the manufacturing process of new cells. Now we can generate virtually unlimited numbers of patient-matched, insulin-producing pancreatic cells.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments