NHS patients' religious services should not be paid for by taxpayer, say critics
NHS Trusts spent a total of £23.5m on chaplaincy services last financial year
NHS Trusts across the UK are spending millions of pounds each year on religious and spiritual services for patients despite objections from the National Secular Society (NSS) that chaplaincy services shouldn’t be billed to taxpayers.
NHS Trusts spent a total of £23.5m on chaplaincy services in the last financial year, according to data obtained from Freedom of Information requests sent to 230 NHS Trusts.
The outlay on chaplaincy services represents an increase of £1.5m on expenditure in the financial year 2012-13 despite the 2011 census showing falling levels of religious belief in the UK.
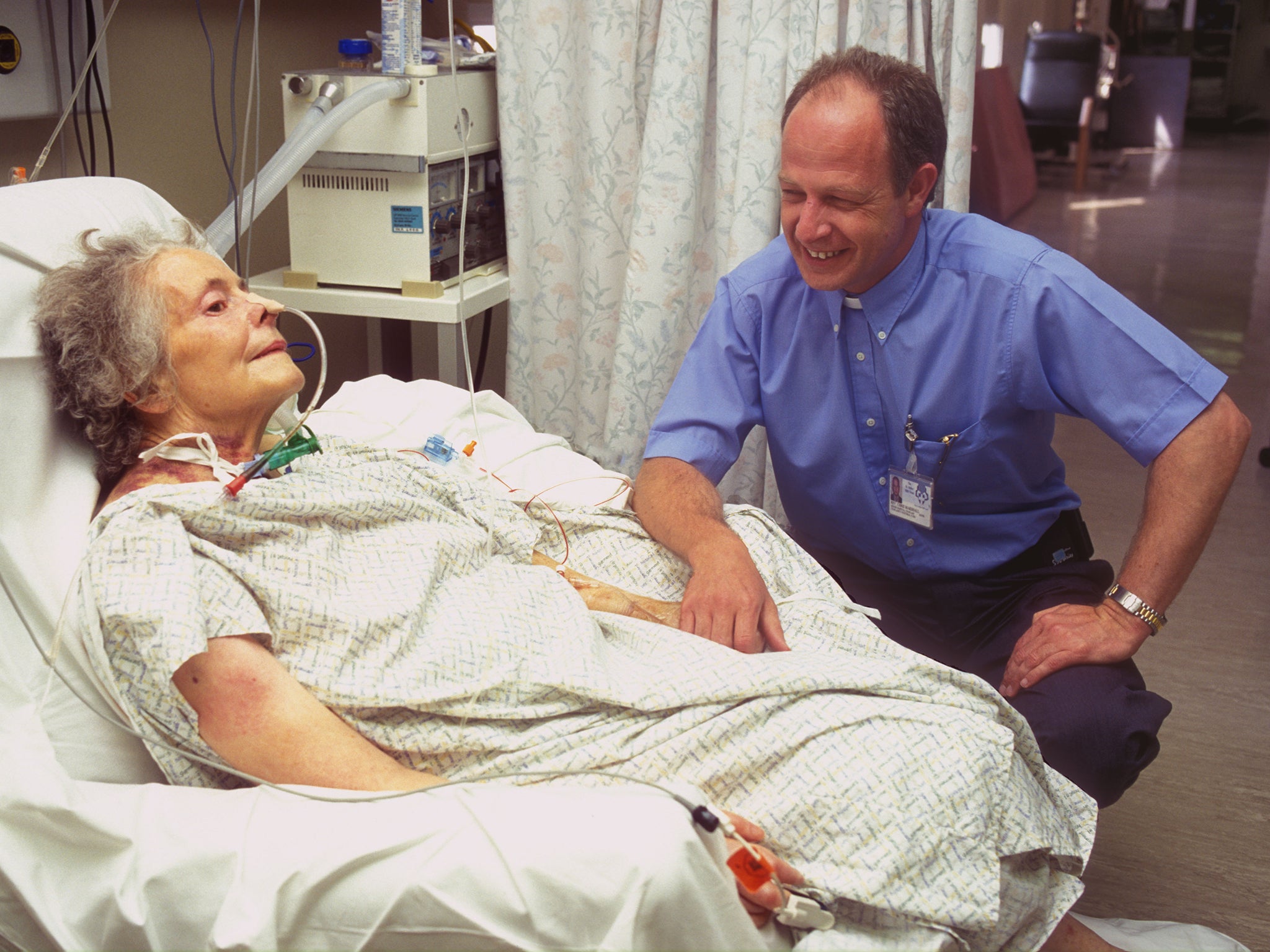
NHS chaplains offer a mix of Christian, Muslim and Jewish services. Their official job description says they “promote, facilitate and administer spiritual, religious and psycho-social care”.
Several Trusts revealed they pay their full-time chaplains from £30,764 to £40,558; part-time chaplains are paid between £25,783 and £34,530. An NHS spokesman said the minimum starting salary for a registered nurse is £21,478.
In addition to employing chaplains, several Trusts pay local religious institutions such as the Roman Catholic Church for extra religious services.
Stephen Evans, the campaigns manager for the NSS, said: “There should be equal access to healthcare and associated NHS services for all patients and NHS staff irrespective of their belief system or lack of one.

“The present system of hospital chaplaincy services leads to unequal care; many patients do not share the particular religion of the appointed chaplain.
“Whether or not chaplains offer their services to all, this is not an acceptable compromise for a large proportion of our diverse society who rightly expect and deserve the state to fund non-discriminatory services. Nowhere is this more important than where people are at their most vulnerable; in a hospital environment. Such services are delivered in a religious context with no alternative provision for the non-religious, who may also appreciate confidential, non-judgemental, emotional support at times of anxiety and distress.
“Rather than pastoral care, what is currently being offered is best described as religious care.
“Religious chaplaincy services could be funded by local charitable trusts, churches or interfaith initiatives.”
Dr Antony Lempert, the chairman of the Secular Medical Forum, argues that the chaplaincy should be transformed from a religious service to an inclusive pastoral service.
He said: “As it stands, chaplains are appointed by religion and are expected to provide religious care, which doesn’t fit within a National Health Service. They should be funded by the religious authorities themselves.
“You cannot provide a chaplain for every belief in a hospital environment, because there are so many religions. There should be generic spiritual support, and then if someone wants a particular religious influence the chaplain is the right person to have the links at hand.”
Only one trust, City Hospitals Sunderland, offers such a service. They employ “spiritual care practitioners”, who support “those who express their spirituality in ways other than through an organised faith or belief”.
However, a Church of England spokeswoman said: “The NHS is committed by its constitution to provide physical, mental and spiritual care to all who call upon its services. For a great many patients, spiritual care is an important component of a holistic approach to health and well-being.
“Through the provision of paid chaplaincy, the NHS is able to access not only the highest standards of professional religious and spiritual care, but also considerable voluntary resources.
“Healthcare chaplains offer extraordinary value for money and enable the NHS to fulfil its constitutional duty of providing spiritual care to all patients who need it.”
Mark Burleigh is Head of Chaplaincy at Leicester General Hospital
“During the day, when we’re not being called out, we routinely visit patients. When people go to hospital, they’re suddenly confronted with their own mortality, and chaplains can be involved in the process of helping them to come to terms with making sense of life in their new circumstances.
“It gives people time to talk about what’s important to them: their spirituality, their sense of purpose in life and how they make sense of the way their illness is affecting their relationships or their future prospects.
“One evening, I was called to a patient who was dying. He told me the story of something he’d done during his military service, which he’d borne the burden of for many years and never told anyone. To me, it didn’t seem like a terrible thing, but to him it was incredibly important and it was causing him distress.
“The following morning, the staff told me that this man had died overnight, but they said he’d seemed much more peaceful after our talk. The family also felt the visit had made a big difference and that they were happier because they felt he was happier."
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks