Radical reform for transplant programme
Hundreds of desperately ill patients are set to benefit from changes to the scheme.
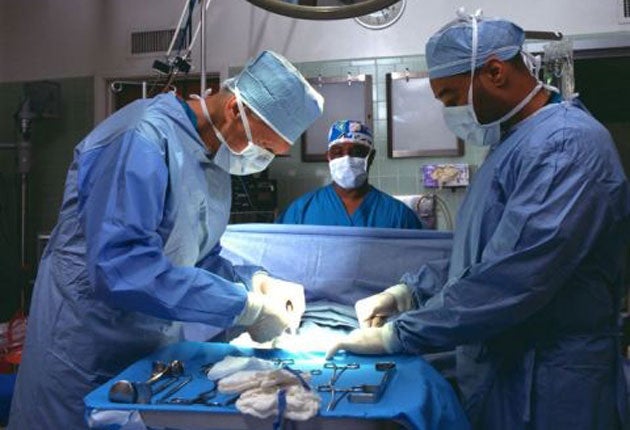
A radical extension to the organ transplant programme is to be launched by the Government in the new year bringing fresh hope to hundreds of desperately ill patients.
In a boost to the existing programme, hospitals will retrieve organs from patients who die in accident and emergency departments – as well as in intensive care units, as they currently do.
The move is expected to make hundreds more organs available to help reduce the lengthening transplant waiting list. A&E departments currently lack the equipment and trained staff necessary for the task.
Figures show that 28 per cent of the population has signed up to the organ donor register, signalling a willingness to donate their organs after death, but that only 1 per cent die in circumstances where their organs can be used.
Most organs for transplant are retrieved from patients who die in intensive care, where life support equipment is available to keep the organs functioning and medical staff are trained to discuss the issue with relatives and carry out the task.
The new scheme will focus on patients brought into A&E with a brain haemorrhage due to a stroke. They are given a CT scan to determine the extent of the brain damage and put temporarily on a ventilator while their relatives are consulted.
In those cases where the outlook is hopeless, relatives will be asked if they consent to treatment being withdrawn and the patient's organs being used for a transplant. Experience shows that when presented with evidence that nothing can be done, relatives are often willing to let their loved ones' organs be used to save another's life.
Only a handful of A&E departments are capable of providing the necessary back-up to arrange the removal and safe preservation of donor organs, but officials now intend to make sure they are all equipped to do so.
There are currently 8,000 people on the transplant waiting list, of whom 500 die annually before they obtain an organ, and the numbers are rising by 8 per cent a year.
The situation is so critical that some transplant specialists are prepared to contemplate extreme solutions, including opening up a legal market in organs. By extending the organ recovery programme to A&E departments, doctors will be able to save hundreds more lives while easing pressure on NHS budgets from the costs of dialysis and similar treatments for patients awaiting transplants. Chris Rudge, the Government's transplant tsar, who is launching the scheme, told The Independent: "During the first few months of next year we will be engaging with more accident and emergency departments in hospitals to help them develop the necessary procedures."
He added: "Approximately 1,550 kidney transplants from deceased patient donations took place three years ago. This year it's probably about 1,850. I think that [increase] can be achieved all over again. Several hundred more patients each year will be able to receive a transplant as a result of this."
Protocols and procedures have been developed in recent months and are now ready to be introduced to ensure the wishes are met of patients who want their organs to give life to others after their own deaths, he said.
"The last two-and-a-half years have seen the most radical changes to the infrastructure that supports organ donation in the NHS. We now have an infrastructure that makes this discussion far more realistic than it might have been four or five years ago.
"It seems to me that a key role of the health service is that if an individual wants to donate their organ after they die and if it's possible to remove and transplant their organs, then it's more than right and proper to make sure that happens on every suitable occasion.
"As long as organ donation is possible it shouldn't matter if you happen to die in an emergency medical department or in an intensive care unit, as long as the circumstances are appropriate. The NHS ought to be doing everything possible to honour that wish whenever it can. The absolutely fundamental reason for doing it is the individual wanted to do it after their death."
The Organ Donation Taskforce, which reported in 2008, set a target to increase transplants by 50 per cent in the five years to 2013. Mr Rudge added: "We've had a 25 per cent increase in two-and-a-half years. Broadly speaking we are on track."
The plan was backed by Tim Statham, chief executive of the National Kidney Federation, who predicted transplant waiting lists would be cleared in three years if the change was adopted.
"We need to get hospitals to accept A&E units as part of the transplant programme. There are seven kidney transplants a day. If we could double it, that's sufficient to end the waiting list," he said.
A spokeswoman for the British Medical Association said: "We've always supported using donors from A&E. We think it's worth exploring. But you have to have teams in place that can retrieve organs very quickly and that needs to be looked at."
Boosting donor numbers: The options
The opt-in
Change the donor register from "opt in" to "opt out", requiring those who object to their organs being used after their death to sign a register.
Pro: People would be much more likely to follow the default position and allow their organs to be used after their death.
Con: It would undermine the "vital relationship of trust" between doctors and patients if doctors could take organs without obtaining specific consent.
Lower the barrier
Retrieve organs from risky patients, eg lungs from smokers.
Pro: Hundreds of people die on the organ waiting list each year. Not all smokers develop lung cancer – it is better to take a chance.
Con: If you spend years on a transplant waiting list and then go through the trauma of an operation the last thing you want is to discover that you have been given a diseased organ.
Legalise the selling of organs
Launch a legal market in organs to boost the global supply.
Pro: High-quality care would be available to donors protecting them from exploitation, illness and death on the black market.
Con: It would be medically sanctioned exploitation of the poor by the rich, and it would increase the risk of donors concealing disease or lifestyle risks.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks