‘They have stolen a decade of my life’: One mother’s fight to find out why her child died
In 2011, Joanne Hughes’ daughter Jasmine died in her arms aged 20 months. More than nine years on, she believes she has uncovered what happened to the toddler, writes Shaun Lintern

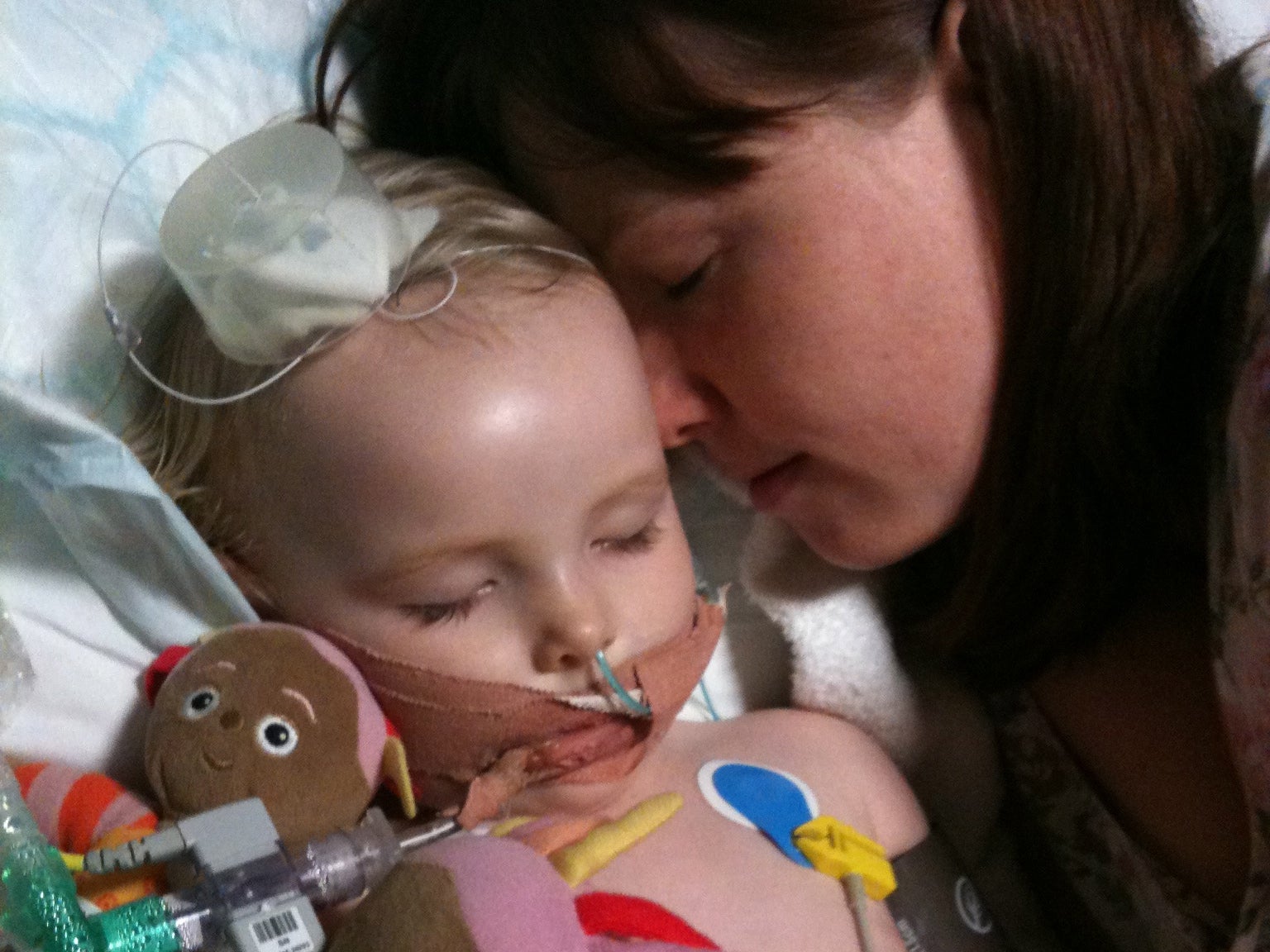
It was while sitting on her bed, surrounded by binders filled with hundreds of pages of medical paperwork, that Joanne Hughes found the note that she believes revealed what had happened to her daughter Jasmine in the crucial days leading up to the toddler’s death.
The 20-month-old had been taken to London’s Great Ormond Street, a world-renowned children’s hospital, in February 2011 after suffering acute disseminated encephalomyelitis (ADEM), a condition that causes swelling of the brain. She died 10 days later in her mother’s arms.
“It was a very peaceful end, we held her close and waited for her heart to stop,” said Joanne, 41. “Then after a while you start to sense that the staff need you to leave because they need to take her to the mortuary and that is just indescribable pain. There’s really nothing more traumatic than having to let your child go.”
It was then, as Jasmine’s life ended, that Joanne and husband Jeff, 49, began their fight to establish what had gone wrong in the care of their first child. The hospital claimed that the death was down to complications from ADEM, backed up by an inquest verdict in 2012. In 2017 Great Ormond Street settled a legal case with the family, but denied responsibility.
So Joanne and Jeff kept searching. In June this year, almost a decade after Jasmine’s death, Joanne was sat at home in Doddington, near Cambridge, scouring hundreds of pages of documents that she had trawled through countless times before. But this time, she found something new – a reference number in a footnote.
It was linked to medical notes made by hospital staff, hidden in 350 complex pages of spreadsheets. She found they contained information that had not been present in the medical records. Analysis by specialist Dr Malcolm Coulthard concluded that they show Jasmine’s death was down to mismanagement of the toddler’s blood pressure at both Great Ormond Street and Lister Hospital in Stevenage, where she was initially treated, causing severe brain damage.
After being given steroid treatment for ADEM, Jasmine’s blood pressure had spiked, Dr Coulthard found. His analysis concluded that, as they attempted to lower her blood pressure, Great Ormond Street doctors then set their target level too low. The combination, he said, caused catastrophic brain injuries.
“When I saw how it described their concerns about her blood pressure being too low and blood supply to the brain my heart was thumping, my face went hot, I started to cry – it was such a physical reaction,” says Jo, who has had three children since losing Jasmine.
“It’s been 10 years of hell, they have stolen a decade of my life but I couldn’t let it go, I couldn’t let Jasmine down.
“What put her in intensive care was avoidable. What was unusual wasn’t her ADEM but how she was managed, and her mismanagement, caused her death, something they have always denied.”
The omissions relating to Jasmine’s blood pressure and treatment from medical records, which should contain all clinical information about a patient, suggested there may have been a “concerted effort” to cover up what happened, according to Dr Coulthard.
He says that some evidence from the computer records, in the CareVue system, does not tally with statements made to coroner Shirley Radcliffe, or was not mentioned at all. Other notes were unable to be provided by the hospitals. The parents believe this was done in an effort to deflect blame, although Great Ormond Street, which describes itself as one of the world’s five leading children’s hospitals, denies this.
“I think it was an active attempt to hide the truth from us. It is impossible that the records that went missing, the records that weren’t provided, the things that aren’t mentioned in the medical notes, the discrepancies with the information provided to the coroner – I just can’t see how all of those things happen innocently in one case, especially when they are all related to Jasmine’s blood pressure management, and the effect it had on her.”
Dr Coulthard agreed to work pro bono for Jasmine’s parents after hearing about what they had been told by the two hospitals.
“My first call with Jasmine’s mother Jo was not long after the inquest. She told me the story and within about three minutes on the phone I realised this was about blood pressures and hypertension. Once I had seen the medical records it was immediately obvious that Jasmine’s parents were not being told the truth.”
He added: “The bottom line is we all make mistakes. Everybody makes mistakes but in the medical profession it is not always encouraged for people who make mistakes to be honest about it and that's always struck me as wrong.

“In my career I’ve tried to be honest and I’ve seen a lot of colleagues being incredibly open and honest. Families value honesty.
“People never get over the death of a child, the best you can do is learn to live with it. And if that process is damaged by a lack of information and honesty, it’s really harmful.”
Remarkably after everything her family has been through Ms Hughes, 41, does not blame the doctors and nurses.
“It’s obviously hard to be able to forgive when a child that you loved so much has lost their life. But we can all as a family completely see how what happened to Jasmine happened. We can all empathise with what the staff must have felt at the time and how horrific that must have been for them.
“I would never blame an individual staff member for what happened to Jasmine.
“Somebody needs to have the guts to actually stand up to Great Ormond Street and my fear is that they are seen as a national treasure; if there’s one hospital in the UK that people don’t want to hear are involved in cover ups it’s Great Ormond Street. That’s why they are able to get away with it.
“Hospitals should have a good reputation when they demonstrate they are open about mistakes, that they support families and staff and that they learn and change.
“For all the cases that do eventually come to light and cause embarrassment, God only knows how many more don’t and that's probably why it persists.”
Great Ormond Street Hospital categorically denies there was any wilful attempt to cover up what happened to Jasmine. It has admitted there were inconsistencies in information and apologised for losing some records and certain information not being shared with the coroner.
The trust has also apologised that Jasmine’s family feel they still do not have the answers they have been looking for and says it is committed to being open and transparent when things go wrong. However, it continues to deny that Jasmine’s blood pressure management contributed to her death.
East and North Hertfordshire NHS Trust, which runs Lister Hospital, has admitted that it made errors in the treatment of Jasmine but refused to accept that the failures in blood pressure management led to her becoming seriously ill.
Jasmine’s parents now want Jasmine’s death to be examined by the Parliamentary Health Service Ombudsman, which has said it is considering the case, and an end to almost a decade fighting for the truth.
“My evenings and weekends have been taken up with this work,” says Joanne. “My other children know this is work for Jasmine but they don’t really understand why.”


Bookmark popover
Removed from bookmarks