Myths and lack of awareness about HPV make women feel ‘ashamed and terrified’, research shows
‘I always describe it as like the common cold that you get on your cervix – most of us are going to get it at some point,’ says doctor
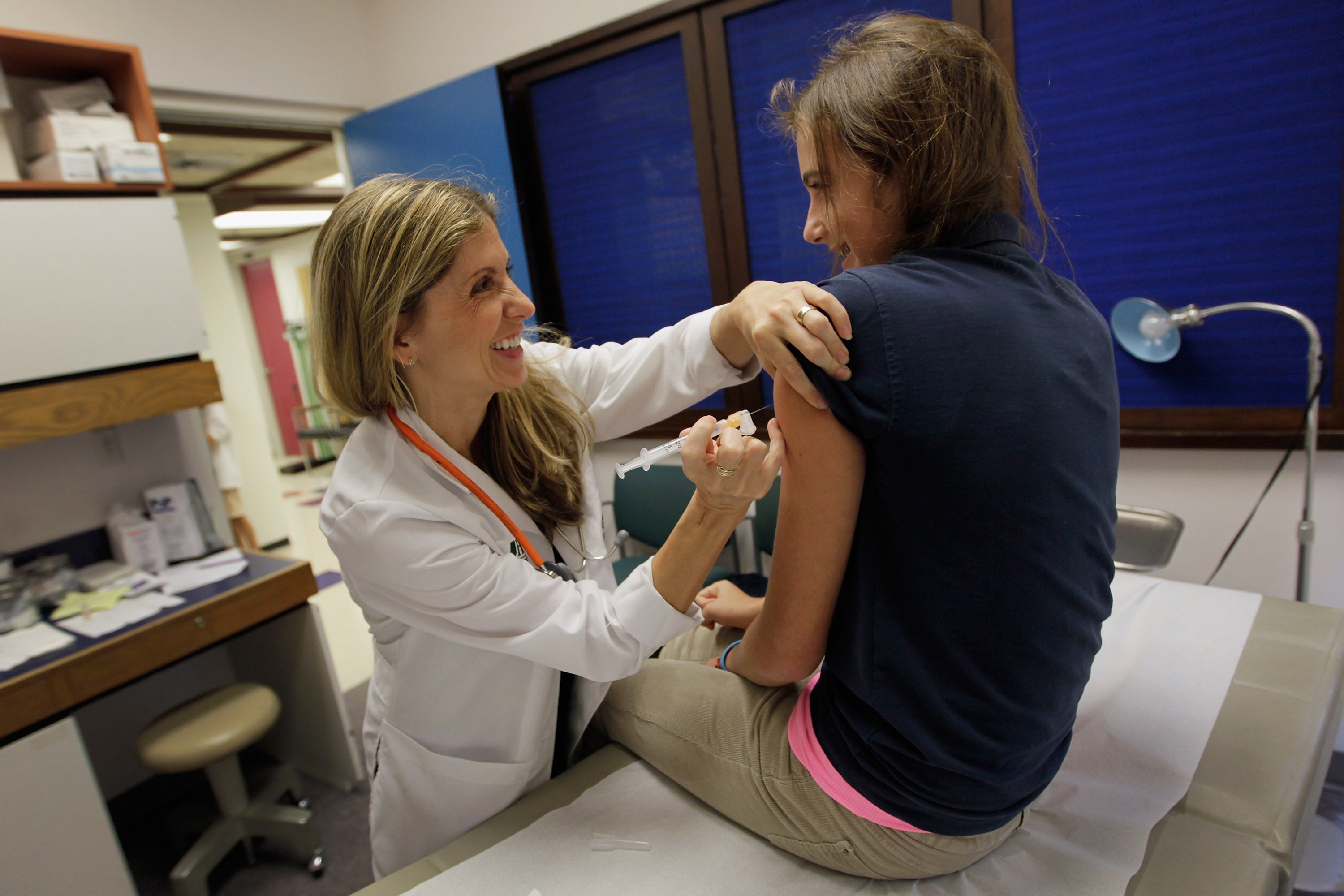
Misconceptions and lack of knowledge about HPV are causing women to feel “ashamed” and “terrified” during cervical screenings, according to new research.
A study, carried out by Jo’s Cervical Cancer Trust, discovered that only half of those who are told they have human papillomavirus (HPV) after a cervical screening understand what the infection is, with many thinking it is more serious than it is.
The vast majority of cases of cervical cancer are caused by HPV – an infection that is very common, and which about eight in 10 people in the UK will contract at some point in their lives, but which can now be vaccinated against.
While it is rare for women to be diagnosed with cervical cancer, with only 3,200 diagnoses in the UK every year, HPV is almost as common as the cold virus. The body generally clears HPV without it causing damage, but a deep-seated stigma about the infection remains.
The leading charity, which polled 857 people who have had HPV, found that more than eight in 10 people who are told they have HPV are frightened they have cancer.
About seven in 10 who were surveyed said they felt anxious, while four in 10 said they felt ashamed. Women routinely say they feel confused, ashamed and terrified, the study found.
Sam Dixon, the chief executive of Jo’s Cervical Cancer Trust, said: “Increasing cervical screening attendance remains vital, but we must not overlook the support that is often required after the test. HPV is so common and yet those affected tell us they often feel isolated.
“We regularly hear about anxiety, worry and even relationship breakdowns because of those three letters. Increasing HPV understanding must go hand in hand with cervical screening awareness so that everyone understands their results, and this very normal thing becomes normalised.”
The charity warned that false notions connecting HPV to sexually transmitted infections can cause concerns about “promiscuity” and “infidelity” – with frontline workers at the charity routinely hearing that diagnoses have caused couples to break up.
Dr Anita Mitra, an academic speciality registrar in obstetrics and gynaecology, said: “I often meet patients who are very scared to receive their cervical screening results telling them they have HPV.
“I always describe it as like the common cold that you get on your cervix; most of us are going to get it at some point, and most infections clear quickly on their own without causing long-term health problems.
“However, if the HPV isn’t cleared it can cause cervical changes, including cervical cancer. And that is why we check for HPV as part of the cervical screening test. It's also important to be clear that it isn't a sign of promiscuity, infidelity or poor hygiene.”
She called for anyone who is anxious to discuss their fears with a healthcare professional so they can help them.
The research found that almost four in 10 said they were anxious about telling their partner they had HPV, and almost two in 10 were scared their partner had cheated on them. And half of all those polled were anxious about sex and intimacy after discovering they had HPV.
Both women and men can be infected, but many women are not aware of this, with the charity warning that because there is no HPV test for men, women are often being burdened with the “emotional strain of a HPV diagnosis”.
The HPV vaccine is now provided to children across the UK and is expected to save many lives.
Cervical screening, commonly referred to as a smear test, helps to pick up early signs of cell changes in the cervix that can turn into cancer.
However, data from last year shows that fewer than three-quarters of all women called in for a cervical screening take up the invitation – with attendance rates for screenings even lower among women of younger ages and those living in more deprived areas.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks