‘Lab-grown red blood cells transfused in to person in a world first’
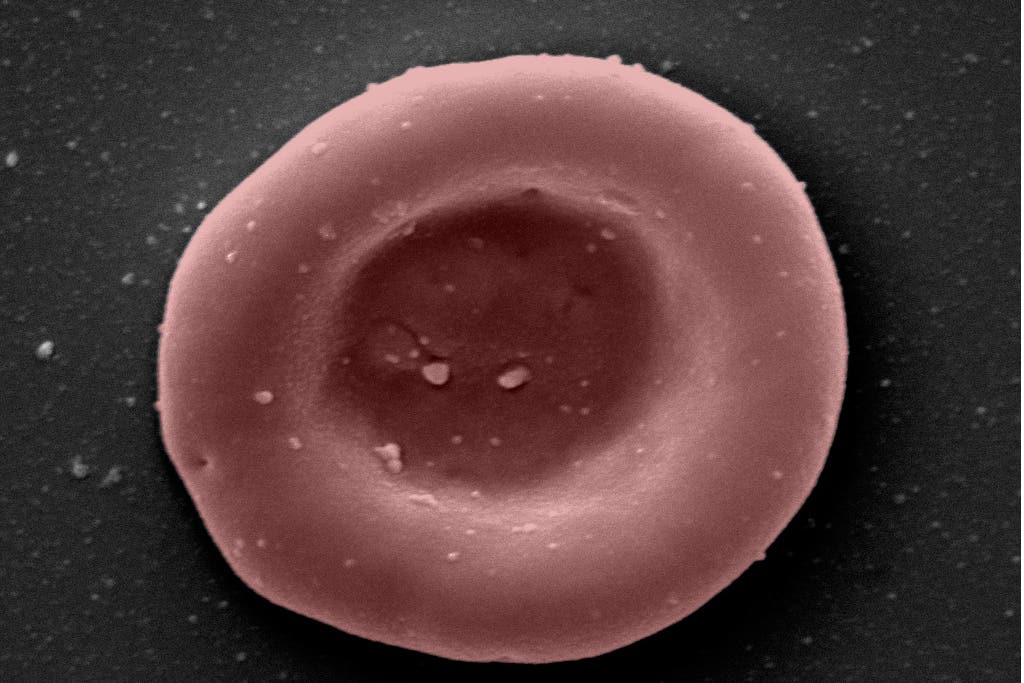
These red blood cells would mean people who require regular long-term blood transfusions could need fewer transfusions in the future.
Support truly
independent journalism
Our mission is to deliver unbiased, fact-based reporting that holds power to account and exposes the truth.
Whether $5 or $50, every contribution counts.
Support us to deliver journalism without an agenda.

Louise Thomas
Editor
Red blood cells grown in a laboratory have been transfused in to a person in a world first clinical trial.
Scientists say that if proved safe and effective, manufactured blood cells could revolutionise treatments for people with blood disorders such as sickle cell and rare blood types.
It can be difficult to find enough well-matched donated blood for some people with these disorders.
This challenging and exciting trial is a huge stepping stone for manufacturing blood from stem cells
But lab-grown red blood cells would mean people who require regular long-term blood transfusions could need fewer transfusions in the future.
Ashley Toye, professor of cell biology at the University of Bristol and Director of the NIHR Blood and Transplant Unit in red cell products, said: “This challenging and exciting trial is a huge stepping stone for manufacturing blood from stem cells.
“This is the first-time lab grown blood from an allogeneic donor has been transfused and we are excited to see how well the cells perform at the end of the clinical trial.”
So far two people have been transfused with the lab grown red cells.
They were closely monitored, no untoward side effects were reported, and the patients – who have not been named – are well and healthy, researchers say.
The amount of lab grown cells being infused varies but is around 5-10mls – about one to two teaspoons.
The manufactured blood cells were grown from stem cells from donors, and then transfused into volunteers in the Restore randomised controlled clinical trial.
The trial is looking at the lifespan of the lab grown cells compared with infusions of standard red blood cells from the same donor.
Because the lab-grown blood cells are all fresh, researchers expect them to perform better than a similar transfusion of standard donated red cells, which contains cells of varying ages.
If manufactured cells last longer in the body, patients who regularly need blood may not need transfusions as often.
Researchers say this would reduce iron overload from frequent blood transfusions, which can lead to serious complications.
If our trial, the first such in the world, is successful, it will mean that patients who currently require regular long-term blood transfusions will need fewer transfusions in future, helping transform their care
Cedric Ghevaert, professor in transfusion medicine and consultant haematologist the University of Cambridge and NHS Blood and Transplant, said: “We hope our lab grown red blood cells will last longer than those that come from blood donors.
“If our trial, the first such in the world, is successful, it will mean that patients who currently require regular long-term blood transfusions will need fewer transfusions in future, helping transform their care.”
Donors from NHSBT’s blood donor base donated blood to the trial and stem cells were separated out from their blood.
These stem cells were then grown to produce red blood cells in a laboratory at NHS Blood and Transplant’s Advanced Therapies Unit in Bristol.
The recipients of the blood were recruited from healthy members of the National Institute for Health and Care Research (NIHR) BioResource.
A minimum of 10 people will receive two mini transfusions at least four months apart, one of standard donated red cells and one of lab grown red cells.
This will allow scientists to find out if the young red blood cells made in the laboratory last longer than cells made in the body.
Dr Farrukh Shah, medical director of transfusion for NHS Blood and Transplant, said: “Patients who need regular or intermittent blood transfusions may develop antibodies against minor blood groups which makes it harder to find donor blood which can be transfused without the risk of a potentially life-threatening reaction.
“This world leading research lays the groundwork for the manufacture of red blood cells that can safely be used to transfuse people with disorders like sickle cell.
“The need for normal blood donations to provide the vast majority of blood will remain.
“But the potential for this work to benefit hard to transfuse patients is very significant.”
Further trials are needed before clinical use, but scientists say this research marks a significant step in using lab grown red blood cells to improve treatment for patients with rare blood types or people with complex transfusion needs.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.