Scientists grow human livers in laboratory
Breakthrough could solve the shortage of organs for transplant and improve testing of drugs
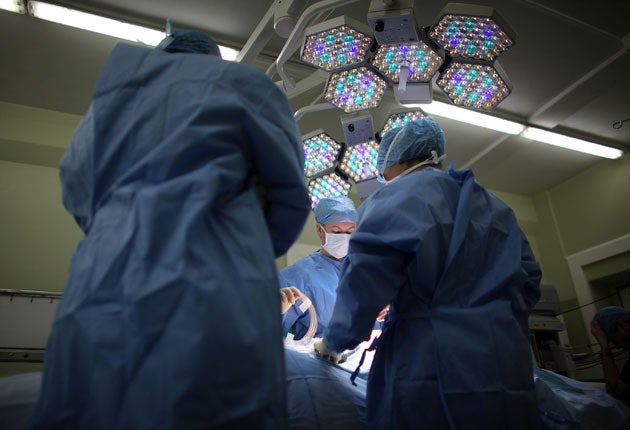
Miniature human livers have been successfully grown in the laboratory, heralding the possibility of customised transplant organs.
US scientists have created working livers the size of a walnut, they said yesterday at the annual meeting of the American Association for the Study of Liver Diseases in Boston.
"We are excited about the possibilities this research represents, but must stress that we're at an early stage and many technical hurdles must be overcome before it could benefit patients," said the project director, Associate Professor Shay Soker from the Wake Forest Institute for Regenerative Medicine in North Carolina.
"Not only must we learn how to grow billions of liver cells at one time in order to engineer livers large enough for patients, but we must determine whether these organs are safe to use in patients."
His colleague, Pedro Baptista, said: "Our hope is that once these organs are transplanted, they will maintain and gain function as they continue to develop."
In developing the procedure, the researchers simultaneously triggered the hope of creating organs on demand and the wrath of opponents of stem-cell research. The technology, which will take at least five years to move from the laboratory to hospitals, also opens up the prospect of growing other replacement organs, including kidneys or pancreases, for patients who are able to donate stem cells.
Artificially grown livers could be transplanted into patients or used to test the safety of experimental drugs. "This would more closely mimic drug metabolism in the human liver, something that can be difficult to reproduce in animal models," Dr Baptista said.
The technique involves removing the liver cells from animal organs with a detergent, leaving behind the collagen "scaffold" and associated blood vesels. These are then seeded with immature human liver cells. The collagen scaffolding gives them shape and structure as they grow, while the blood vesels, attached to a "bioreactor", provide oxygen and nutrients and take away waste products.
Laboratory livers that were nourished in a bioreactor for a week began growing and functioning like human organs, they said. Scientists at Massachusetts General Hospital in Boston used a similar scaffold technique earlier this year to build miniature rat liver grafts to transplant into live rats, which survived for several hours.
Liver disease is the fifth biggest killer in England and Wales, after heart disease, cancer, stroke and respiratory disease, and the only major cause of death that is still increasing year on year.
Some 16,087 people in Britain died from liver disease in 2008, a 4.5 per cent increase on the previous year, and the number of deaths is predicted to double in 20 years. Some 644 livers were transplanted last year, while 1,121 patients were on the waiting list during 2007-08. The two main causes of liver damage are alcohol cirrhosis and hepatitis C infection.
Sarah Matthews, a spokeswoman for the British Liver Trust, said: "Technology such as this is much needed. Currently [organ] supply isn't meeting demand, and for every one person who receives a liver transplant, 10 people die.
"Expanding waistbands and heavy drinking habits are having an impact on the quality of donor organs available in the UK, therefore we desperately need developments in liver science. We are encouraged by these results but would also like to warn patients that this technology is a good few years off from becoming available," she said.
Professor Mark Thursz, the medical adviser to the British Liver Trust who attended the Boston meeting, said: "There are now two or three groups of researchers working on this type of de-cell, re-cell system to create an artificial liver, and the results are encouraging.
"The report suggests that the authors have overcome one of the major hurdles in creating an artificial liver, to generate functioning human liver cells in a 'natural' liver structure."
Hope for those waiting for a transplant
David Kallin, a marketing consultant living in London, has been waiting for a liver transplant after being diagnosed with a blocked portal vein in March, following complications from intestinal inflammation and Crohn's disease.
He said: "My portal vein, the key channel of blood and oxygen between the heart and the liver, is completely blocked with blood clots. My gall bladder is inflamed and my spleen is enlarged because lesser veins are having to cope with too much blood flow. It's dangerous because if they were to burst it could lead to internal bleeding, which can be fatal. There's a bad myth that anyone who has a liver problem has brought it on themselves.
"I am living in limbo. If there was a stockpile of livers, at least I would know where I stand. I would prefer an operation now as I could recover in a few months and be living a new, normal life. At the moment, there's this massive caveat that sits above my life and I can't make too many plans.
"We shouldn't halt the progress of science. Scientists have to 'play God' – not to be bloody-minded, or to create some super human race: it's progress. And the sooner the better."
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks