‘It’s meaningful work’: The doctor who performs euthanasia in Canada — and the doctor who refuses
In Canada, euthanasia is known as medical assistance in dying — or MAID — and in 2023 it will become accessible for people who solely have a mental health condition. Holly Baxter speaks to two physicians on opposite ends of the spectrum: a MAID assessor and a conscientious objector

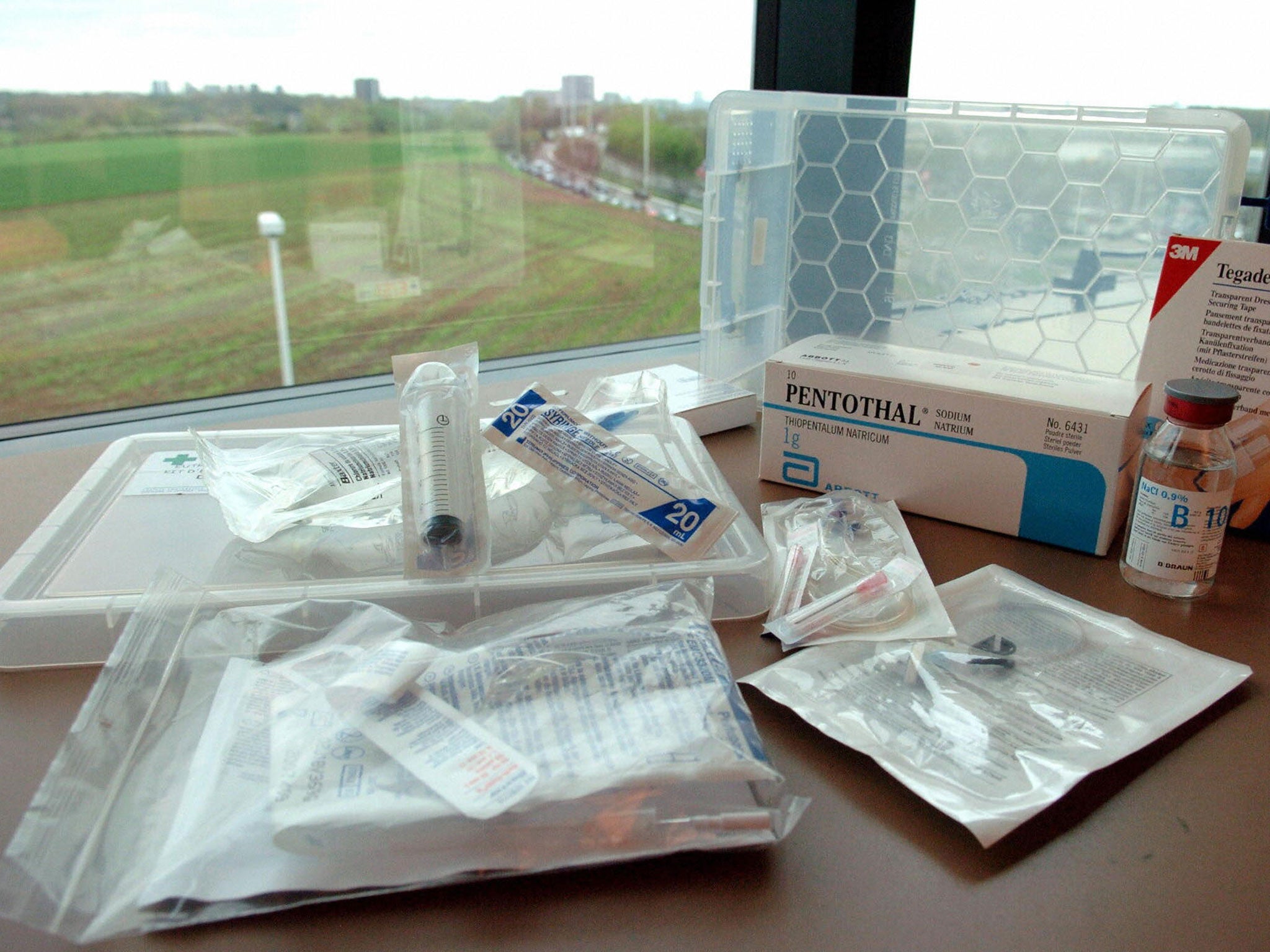
It was everyone’s worst-case scenario. When retired corporal and Paralympian athlete Christine Gauthier spoke to a veterans affairs officer on the phone about installing a stairlift in her home, she says, she was offered euthanasia instead.
“I have a letter saying that if you’re so desperate, madam, we can offer you MAID, medical assistance in dying,” Gauthier told a Canadian House of Commons veterans affairs committee in early December. The 52-year-old had lost the use of her legs after a military training accident in 1989 and is a five-time world champion para-canoeist. She wrote to Prime Minister Justin Trudeau after the alleged incident with the government worker to express her concern at how euthanasia in the country, which has been legal since 2016, is being handled.
The story seemed to take an even darker turn when Canada’s veterans minister, Lawrence MacAuley, said that multiple instances of disabled veterans being offered euthanasia equipment by a government employee had been referred to the police. This was not an isolated incident or a singular misunderstanding. However, all cases did involve one single employee, who has since been suspended.
Many will find it reassuring that a rogue employee — rather than the systemic devaluation of disabled lives — appears to be behind this shocking offer. But others argue that the problem can still become systemic very quickly. When assisted suicide is under the purview of the government, a singular, nefarious individual can do damage on an unprecedented scale. Is it worth it?
When euthanasia — or MAID, as it’s more commonly known — was made legal in Canada in 2016, it was for terminally ill people only. In 2021, MAID was expanded to people who are not necessarily terminal but who are living with debilitating, incurable pain caused by a physical illness (referred to as “a grievous and irremediable medical condition” in Canadian law). In March 2023, that definition will be expanded to include people with mental illnesses. And though there has been much online scaremongering — especially among right-wing tabloid media — about “children” becoming eligible, there are no plans for minors to feature in Canada’s assisted dying program yet. However, the question of whether “mature minors” — most likely 16 and 17-year-olds who are terminally ill — should be allowed to access MAID is currently being studied by members of the Canadian parliament, whose report is due to be delivered in February.
Importantly, conscientious objectors are allowed under Canadian law. No doctor, nurse or pharmacist whose personal beliefs go against euthanasia can be forced to partake in it. It is legal to refuse to prescribe or administer MAID.
Dr Ramona Coelho is one of those conscientious objectors. A family medicine practitioner based in London, Ontario, she has spent most of her career working with vulnerable and disabled patients. For her first five years as a doctor, she did “halftime home care”, which involved administering to “people who had dementia or severe disabilities, people who were struggling with addiction or others who needed me to come to their house” rather than being able to make it into a clinic. “I would say that I was a little bit naive going into it,” she tells me, over a video call. “I didn’t understand how a lack of resources can really increase suffering.” She worked with chronic pain patients and the severely mentally ill, “a lot of refugees, men who’ve been through the penal system”.
“Through my career,” she says, “I’ve seen long suffering caused by a system that deprives [such people] of, and delays, their recovery.”
When MAID was first brought in, under its initial guidelines for the terminally ill, it didn’t affect Dr Coelho’s practice much at all. But in 2020, when it was announced that euthanasia would soon become available to the long-term disabled who were not at risk of imminent death, everything changed. To her, it was clear that a government-run healthcare system couldn’t be trusted to implement MAID at the same time. Her vulnerable and disabled patients already faced extremely long waiting lists for occupational therapy, certain specialists, and social care. Rather than investing into making those systems better, what was stopping the government from instead aiming to cut waiting times by proactively offering her most complex patients medical assistance in dying?
“This is actually happening,” Coelho tells me. “People are on waiting lists for specialised mental health care for five years.” (The Canadian Institute for Health Information’s report on mental health services in 2021 found that one in 10 Canadians wait four months or longer for access to care.) She saw suicidal patients with intractable depression who would express the desire to die but who she knew would actually improve if they could access appropriate care. She knew from all the medical evidence available that most people who express suicidal ideation — including nine out of ten people who attempt suicide — will go on to live normal lives and will not want to die in the future.
“You look at [heart attacks], concussions, brain injuries, spinal cord injuries, strokes — big, big diseases that are often a setback and might lead to disability in a patient. They have increased suicidality while they’re adjusting, but [after two or three years], the overwhelming majority rate their quality of life the same as an able-bodied individual,” Coelho says. She adds that often, physicians are simply too ableist to imagine a disabled person living a happy and fulfilled life even after sustaining life-changing injuries: “What I’ve encountered that I didn’t realise is the kind of biases that can play into thinking someone must be suffering intolerably and they won’t get better. And I’m speaking from personal experience — I used to take care of these people with severe disabilities as a young and inexperienced doctor. I would say that probably, a lot of the time, I was suffering more for them than they were suffering themselves. And it took time to realise that they actually enjoyed life… It was like, I did not understand disability. And the average Canadian does not understand disability.”
Coelho claims that she often comes across physicians who don’t think her patients’ lives are worth living. She describes a disabled patient who went to the hospital with “totally curable pneumonia,” whose doctor thought it might be best to leave to die rather than administer antibiotics. Another patient, she says, was proactively offered MAID when he wanted to discuss increased home care funding. The cases that do make it into the headlines — like Christine Gaultier’s — Coelho claims are just the tip of the iceberg.
What especially alarms Coelho is the expansion of MAID to those who are suffering only from mental illness, as is planned for 2023. “When you look at mental illness, there is no guidance to predict who will get better,” she says. Despite the work of psychiatrists and many thousands of medical papers, it still seems that it’s all down to chance: “So if you think about cancer, for example, we have some understanding of the prognosis over time. And someone can outlive their prognosis or not live up to their prognosis. It’s a prognosis, but there is some kind of predictability. We have no such standard in mental illness. So it really will be guesswork.” Coelho brings up the case of a long-term mental health patient of hers: “She was hospitalised for a year. She’d had electroconvulsive therapy, I can’t remember how many times. She saw many, many specialists over many, many months. I know that probably at some point, I was losing hope, and she was losing hope — we were losing hope together, though it’s not something that I ever voiced. But now, she visits her grandkids every week, she volunteers at the hospital… and she’s doing really well.” This patient reflected on the mental health expansion to MAID recently and said to Coelho: “That would have been me, wouldn’t it?… I think they would’ve given me MAID.” Coelho pauses, then adds, “And I said: yeah, that’s exactly right.”
Coelho isn’t impressed by the arguments of her fellow physicians who support medical assistance in dying: “They’re just saying autonomy is everything and that’s what the patient wants. They want it. But it’s a very limited way to look at choice.” She believes that hand-waving about personal autonomy is meaningless when patients are vulnerable and at the mercy of an overstretched healthcare system: “You could say it’s a choice, but is it really a choice if you’re waiting for two years to get access to a service and you can get MAID in 90 days and you’re feeling quite desperate?” She thinks that the very existence of MAID lets the government off the hook: “I don’t think we should be offering death as a solution for life’s suffering. I think we should be working on improving our social policies.”
Indeed, Coelho doesn’t believe euthanasia can ever be responsibly applied, and now believes it should be banned entirely, even in cases of terminal illness. “I understand there’s some very sympathetic cases, but the thing is we always have to worry about the population. If one person dies on their own terms, but another group of people don’t, and actually are wrongfully killed because of our system, then that’s not a viable system.” She doesn’t deny that some people would benefit from retaining MAID, but believes that they are in the minority, and that the damage done to society isn’t worth it: “Here you have this group of very wealthy, privileged people who want to die on their own terms. And you have another group of people who are marginalised who will be affected by these laws.”
Dr Stefanie Green is a Vancouver-based physician, a MAID assessor, and the author of This is Assisted Dying: A Doctor’s Story of Empowering Patients at the End of Life. She has been working on the front lines of medical assistance in dying since it was made legal in Canada six years ago, and is all too familiar with the negative press that often concerns her work. One such story that made headlines a few weeks before we speak is that of an Ontario man who said he was considering MAID because he was facing homelessness. Amir Fasoud, who is 54 years old and disabled, said that he had lost the will to live after facing unrelenting financial hardship following a back injury that forced him out of work. After a $60,000 GoFundMe was set up in his name by a well-wisher who had read about his case in the news, Fasoud said he was no longer considering applying for MAID.
“There are reports of people saying, I’m going to become homeless and therefore, rather than live on the street, I would rather have MAID,” Dr Green tells me. “That doesn’t mean you’re going to be found eligible for MAID… and I think it’s important to know that because it’s easy to put your hand up and say, ‘Well, I want to jump the queue. I am going to have MAID if I don’t get that appointment at the pain clinic. They told me it’s a three-year wait, but I can get MAID in six months.’ It doesn’t work like that. A) You don’t get it in six months, and B) that doesn’t mean that you get MAID at all.”
Green is extremely familiar with the timescales and the processes involved in MAID; her day-to-day life involves working with these intricacies. She believes that the promotion of stories like Fasoud’s — upsetting as they may be — oversimplify the issue. MAID guidelines are stringent, she says, and almost every instance of medical assistance in dying concerns someone with a terminal illness who is nearing the end of their natural life. What is it like, I ask, being the doctor who someone relies on for MAID?
“It is — what’s the word? It is extraordinary,” Green says. “And it’s always unique. Every person and every person’s situation, and every person’s reasoning and every person’s circumstances are always different from someone else’s. Just like every birth is different… Laws are meant for generalities. Clinical work is for individuals. So what is it like? It’s intense. It is often emotional. It is often surprising. And it is important to remain patient-focused. So what’s meaningful to the patient — to the person — is what has to become what’s most important in the event itself.”
Like any big family event, Green adds, planning a person’s death alongside their loved ones can be logistically and emotionally complex: “It’s challenging to bring in loved ones and families. I mean, the majority of the time they are rallying around and supporting the patient, their loved one, but not always. It can be challenging to manage family dynamics, faith-based dynamics, unforeseen circumstances. All these things occur. But I have to tell you, even looking at last year’s data, 97.8 per cent of all assisted deaths in Canada were for patients on what we call ‘track one’. These are people who have a reasonably foreseeable death. The vast majority of them have a cancer diagnosis. The vast majority have family support. They go through the rigorous process, they make this request, we help them.” (Canada’s third annual report on Medical Assistance in Dying shows that only 2.2 per cent of people who accessed MAID in 2021 — 219 individuals — were not terminally ill; 65.6 per cent had cancer.)
“As a physician, people come to me and ask me to do things they’ve never asked of anyone else,” Green continues. “They tell me things, they tell me secrets. It’s very, very privileged work. And to be able to facilitate someone’s final wishes — to be the one who’s asked, and to be able to give it to them — is incredibly meaningful work. That’s what it’s like. It’s meaningful.”
Does being present at so many people’s deaths change Green’s perspective on life, I ask? She has an immediate answer. “How can I not? How can I not project myself into the situations I encounter? I see someone roughly my age in a certain circumstance — how can I not think about what I would do in that situation? Who would I want with me in that situation? Would I want my pet with me or not? It can be as superficial as that to the much more deep. And so when I have those little drives home afterwards, when I think about those issues, I become much more reflective about my own life and how I live it, and how I want to live it, and who’s important to me, and whether I’ve told them that recently. It makes me a better doctor when I do that. It certainly, I think, makes me a better person, makes me a better wife, makes me a better mother.”
I ask Green whether she thinks that MAID could be an easy out for a government that would rather not spend more on resources for vulnerable populations. “I mean, of course there are grossly inadequate resources for some of our population,” she says. “We need better community-based mental health services. We need better community-based palliative care services in some places. We need better disability supports in our communities. We need lots of things that we don’t have. We’d love an MRI machine in every county hospital. We don’t have that either. There’s resource issues and they have worsened during the pandemic.”
Green recognises the importance of campaigning for more medical funding, but also thinks patients should be taken seriously when they weigh up the realities of their own lives in context: “Suffering is one of the eligibility criteria for MAID… If a patient is in a situation where they have very limited access to very limited resources or they can’t access them at all — it’s only in the big city or it’s a three-year wait or it’s not available altogether, it’s only in a specialty clinic in London, England because they have a rare disease — what you’re asking is whether we should tell them that they need to continue suffering even though they can’t access those services, or whether maybe we recognise that they understand their situation and their suffering better than anyone else does. And respecting that and knowing that and seeing that they have the capacity to make their own decisions in their life about their healthcare.”
For Green, it comes down to a human rights issue. “It feels very uncomfortable for some members of society,” she says. “They say, okay, really what we should be doing is giving them better resources. That is absolutely correct. We should be giving them better resources. But we can’t do that by removing other rights… We need to not hold individuals hostage to society’s failings.”
Green is aware that many people feel uncomfortable about MAID being made available to mature minors, or to people who are solely suffering from mental health conditions. But she sees medical assistance in dying as a normal part of medicine, subject to the same rules and regulations. Opening up MAID to such patients follows a normal precedent, she says, rather than being the work of some radical sect of euthanasia expansionists: “We already have precedent in our country for mature minors to make life-or-death decisions about their own healthcare. They’re allowed to decide whether they will or won’t receive blood products, for instance, if they’re Jehovah’s Witnesses… And the question is: Will we extend that to the decision about MAID?… It’s a reasonable discussion to be having in our country, and I expect we’re going to have it, but to date it’s not allowed. And it may or may not come to our country at some point. So onwards with the debate, I say.”
Nor is Green worried about the 2023 changes which will allow people who solely have a mental health condition to apply for MAID. She reminds me that people who have mental health conditions combined with physical health conditions have always been eligible, and have applied for and accessed MAID over the past six years: “We have six and a half years of experience of assessing and providing for people with mental health disorders and concomitant physical illness…. Can we differentiate between a rational, fact-based, well-informed requested for assisted dying versus a suicidal ideation or a suicidal mental health patient requesting death? I would say clinicians can do that. I think we are trained to do that. We have been doing that for decades. We know the difference between a rational request for an assisted death and suicide.”
Green speaks of a supportive environment among her fellow physicians and her fellow Canadians when it comes to MAID: “Don’t forget, the vast majority of Canadians support this — well over 80 per cent, consistently.” (A 2022 survey done by Dying with Dignity showed that 86 per cent of Canadians support MAID provisions, which is the same percentage as in 2021.) Indeed, she says she is often “overwhelmed by the level of gratitude” from patients and their families. But she’s aware she has her detractors, and sometimes they can be scary: “I hesitate to say this too far out loud. I’m not looking to make myself a target. But I’m not looking to hide, either. I’ve done it very openly and very transparently from the first day I’ve done it, and I will continue to do so. Do I get hate mail from time to time? Sure. Do I get people heckling me at public events? Sure. Do I expect that to ramp up with the rhetoric that is whipping round the media these months? Unfortunately, I do. I’ve seen that rise from some of my colleagues. We’ve started to collect these events and document them and report them. And we are seeing a rise in the most scary tactics. But I won’t focus on that. I guess, at this time, it’s an unfortunate reality. Doesn’t need to be.”
I ask Green what she thinks of physicians who, like Coelho, conscientiously object from MAID. “She has every right to not do this work or participate in any way,” she says. “I fully respect that. Absolutely. I would fight for her right to that… I do hold people to professional standards. If you’re a clinician and someone’s in your office and they’re asking for resources, if you don’t want to do that work or can’t do that work, you just need to make sure someone answers their question.”
And what about people who stand vehemently against euthanasia because they think its very existence means the government won’t provide appropriate social resources? “I am willing to stand next to that person with a bullhorn and scream for more resources. I’ll bet you today’s salary that person will not stand next to me and demand more resources with me because… I think some people in that situation might be more interested in opposing MAID than demanding social resources. So, the door’s open to work together. Please, I’d be happy to lend my support and my voice to the call for the need for more social resources. I couldn’t agree more. I can’t do my job and offer resources to patients and figure out whether they’ve given serious consideration to them if those resources don’t exist.”
I mention that I spoke to a physician who believes MAID should be banned entirely, because it can never be responsibly applied. What would I say to such a doctor, I ask Green? “I would say: Who is she to decide for that person whether it’s worth it or not?… Let’s let the patient in that situation, who knows themselves, what it feels like, what their value system is, what’s important to them — let’s let them decide. Let’s not leave it up to the palliative care doctor to decide whether they’ve got two weeks left to live or not.” Green describes a situation, common in hospices and hospitals across the world, where people at the end of their lives are sedated to the point of unconsciousness without being consulted: “[The doctor thinks], they are suffering intolerably. I will sedate them, so they are not conscious of their suffering… By the way, I didn’t consult the patient. I might have consulted their family. There’s no oversight, no law, no reporting, no accountability, no idea how often it’s happening. And yet how can that be okay? Whereas asking the patient to make an autonomous decision with all the facts, in conjunction with a clinician, often in conjunction with family — how can that not be okay in the same situation?”
Green believes in the ability of her patients to make informed choices to the end. “How about we let the patient decide?” she says, addressing the imaginary anti-euthanasia doctor in the room. “Who are we to say that they can’t? They are capable human beings. You do you; let’s let them do them.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks