As a paediatrician, I can tell you that the case of Charlie Gard isn’t as black and white as it seems
I have been in several situations where I have had to discuss the recommendation to switch from active to palliative treatment. No parent ever wants to have to make that decision
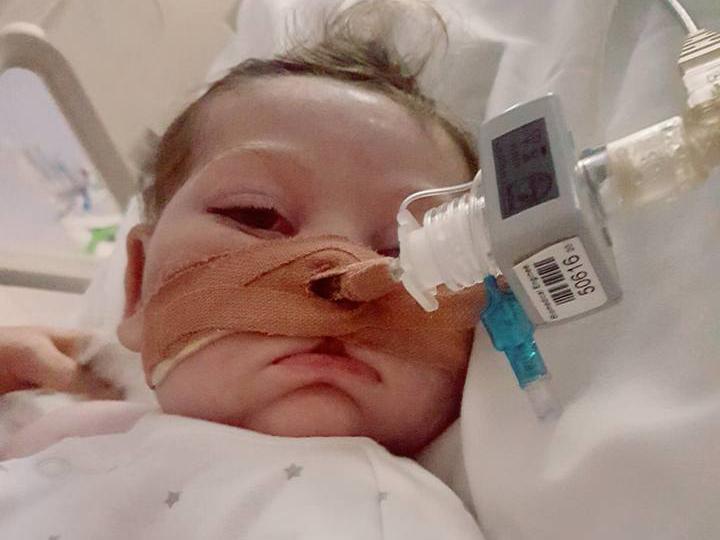
Some will agree and some will disagree with my musings on Charlie Gard, but I hope this piece will highlight that these situations are never as simple as you may think from the news.
Charlie's story has been all over both traditional and social media in the last few weeks. For the few of you who may have missed the details, he is a baby with a very rare genetic condition. The cells of his body can’t use energy appropriately, leading to his organs and muscles being unable to function properly. For the last eight months he has been kept alive by technology on the intensive care unit at Great Ormond Street Hospital (GOSH) requiring round the clock intensive care. There is no known proven cure for his condition but at the moment he is stable and could, in theory, be kept alive for an indefinite period of time.
After months of deliberations and a battery of repeated tests and examinations, the medical team at GOSH are completely convinced Charlie has no chance of recovery. Thus they want to withdraw treatment and switch to palliative care i.e. managing any pain and distress whilst nature takes its course. Their tests done at GOSH have been suggestive of irreversible brain damage. In the opinion of the professionals at GOSH, Charlie will never breathe unaided, or swallow food, and he has little or no awareness of the world around him. He cannot see, hear or feel. He also reportedly has fits that are difficult to control. Charlie's parents refute this and are convinced Charlie responds to their voices and touch, and that he has far more awareness of the world around him than the professionals believe. They do not accept the view of the professionals at GOSH that his condition is irreversible.
Charlie’s family searched all over the world for potential cures and identified a doctor in the USA who suggested that an experimental treatment called nucleoside therapy might offer some chance of stopping further deterioration of his condition; it is unclear as to whether this doctor feels this treatment could actually reverse his symptoms. This treatment has never been used on any human being with Charlie’s condition, although it has been used on children with similar mitochondrial diseases. There are also potentially side effects that could cause more harm than benefit.
Because there is no hard evidence that this treatment might help, and the medical opinion is that Charlie’s brain is damaged beyond any repair, the team at GOSH feel that it is not in the best interests of Charlie to transport him to the USA, that the risks far outweigh any potential benefits and ultimately the treatment would be futile, merely serving to prolong his suffering.
Charlie's family disagree. They created a huge social media campaign, assembling “Charlie's Army”. Their dreadful plight whipped up huge amounts of sympathy from the general public, playing to the idea of every parent’s worst nightmare, fighting heartless NHS medics to save their boy's life. They have crowdfunded enough money, over £1.2m, for him to be taken to the USA for this treatment. However, due to the complete lack of common ground between the medics and the family, Charlie’s case went to court and, after spending a lot of time weighing up the arguments, a judge ruled that Charlie should have active care withdrawn. His parents then appealed to the Supreme Court who ruled in favour of GOSH’s view. His parents then went to the European Court of Human Rights in Strasbourg who agreed with the previous judgement. As things stand at the moment, the doctors at GOSH legally have the right to switch to palliative care, but there is still debate as to whether he should be allowed to die at home or in a hospice.
The fundamental question here has to be about what the longer term expectation for Charlie is. If the outlook is dismal and his brain is not going to recover to the point where he will have any meaningful awareness of the world around him, and he will never be able to live independently of machinery, what possible good can come of prolonging the inevitable? However assessment of his brain function is the difficult one. He will already have undergone numerous objective assessments of his brain including MRI scans and electrical tests, and these are the best measure we have to work out the answer. Charlie’s parents disagree with the neurologist's opinions; I can only begin to imagine the agony they must be going through at being told that nothing more can be done, and their son is going to die, when they are convinced that the medical assessment of Charlie's brain function is flawed. What parents would not try any treatment, whatever the risks, and however slim the chances of it working, to keep their child alive?

I have been in several situations in my career as a paediatrician where I have had to discuss the recommendation to switch from active to palliative treatment. No parent ever wants to have to make that decision; I have never expected parents to make that decision without having adequate time, information and discussion, however long that takes. I have been lucky enough till now to have been able to find common ground and for joint decisions to be agreed as to which way to go. With time and open, honest discussion, doctors can understand parental viewpoints and vice versa. This is never easy for families but don’t believe that this is ever easy for the medical teams either. We are human too and I have shed tears many many times.
It is sad to hear about cases that end up having to go to court; I wonder how the gulf of understanding between the families and the teams looking after their children has been allowed to open up. A judge’s decision on what should happen is an unsatisfactory outcome for everyone compared to a plan negotiated and designed together. A verdict for care to be withdrawn means the parents will grieve for longer and will maybe never find resolution. If care is to be continued then medical teams will be going against what they believe to be ethically correct.
The other big issue in Charlie's case is the potential treatment in the USA. At first glance it seems a no-brainer; if it is the only hope then go for it, what is to be lost? But as ever it is more complex than that. There are inherent risks to life in transporting a critically ill child across the Atlantic aside from the expense. If hypothetically the treatment proposed had a 90 per cent chance of success and the risk of side effects was negligible then maybe that trip would be worth the risks. This view at GOSH is that it would be a treatment with at best a chance of stopping any further deterioration; it is not going to reverse his condition or cure him and any potential side effects in Charlie’s situation are unknown. The decision made in the court hinged around weighing the potential benefits against the potential risks and the judgement suggests that the risks outweighed any potential benefits.
Comparisons have been drawn between not trying experimental chemotherapy in childhood cancer. This is different as in such situations there may be a chance of reversing the condition, and even so the child’s level of brain function would need to be assessed. If a child had severe brain damage to the extent that they were dependent on intensive care, it is likely that the treatment would not be given as the long-term outlook would be poor regardless.
As adults, we can write living wills outlining the limits of intervention with which we would be happy if we were critically ill and unable to articulate our wishes. For sick children those decisions have to be taken by parents who then have to live with the consequences of their choices, as do the medics. It is hard to be objective as a parent, and medical teams always try to work together with parents to do what is more right than wrong. It is still sad even when this works; but sadder when common ground can’t be found and the law has to become involved. To read much of the media coverage, one would think that the medical team were heartless ogres and just wanted to give up. It is always important to look at the bigger picture and ask the fundamental question that often gets forgotten in the emotion – what is in the best interests of the child? Not of the doctors, the nurses or even the parents; but of the child. Technology can keep human beings alive for a long time but there is more to being alive than a machine inflating your lungs and a tube feeding you into your stomach or veins. Quality of life, dignity and humanity all need to be taken into account; it seems these factors get lost all too often.
Many arguments have been made that life should be prolonged at all costs; I fundamentally disagree with this having seen many children over the years where, in retrospect, all that was actually achieved was prolonging the process of dying. Medical teams have been accused of “playing God”; I would contend that the act of intervening in any illness could be interpreted as playing God including what is currently being done actively at GOSH.
In situations such as this, the media have a field day. The medics are inevitably portrayed as cold-hearted self-appointed deities whilst the families are depicted as the victims of an uncaring health establishment that only cares about money and itself. It is a scenario that sells papers and appeals to that most basic human emotion of compassion.
The reality of these situations is never as black and white as what you will read over your cornflakes. The medical arguments will never be articulated in any detail, both because of their complexity but also because of issues around patient confidentiality. They can also seem very dry in comparison to the grief and anger of families.
As human beings we like things to be black and white, good guys versus bad guys, the establishment versus the little man. Unfortunately medicine inevitably operates in shades of grey and there is rarely a 100% “right” thing to do. Every decision is a balance of potential benefit against potential harm; even popping an ibuprofen for a headache is a calculated risk between easing a headache or getting horrendous heartburn. In situations such as Charlie’s, the medical teams involved will have relentlessly weighed up the potential benefits of continuing to keep him alive using artificial means and transferring him to the USA for an experimental treatment against the risks of transporting him there and the chances of this course of action having any significant beneficial effect on the long-term outcomes.
As a result of the binary media coverage, many people have developed fixed opinions on the situation on one side or the other, which they express passionately and loudly. The fact that people with as high a profile as the Pope and the President of the USA have become involved reflects how emotive this has become. Clinical staff at GOSH and anyone who expresses an even slightly contrary opinion (myself included) have been abused and insulted on social media when ultimately everyone involved genuinely believes that they have Charlie’s best interests at heart.
That his parents would want to try any means possible to find a way to improve things is beyond criticism; in fact I would argue that if parents did not consider this it would be abnormal. However, parents need to be able to make informed decisions and consider all the shades of grey, and it is disappointing to see how much of the media have portrayed this as a black and white issue without really representing all of the facts objectively.
As for Charlie, the situation has reached a level of unprecedented public interest. World leaders are involved. The Pope has offered for his care to be continued in Rome and President Trump has intimated he would support him coming to the USA. Who knows what the outcome will be? But everyone involved must learn from this, so that the Charlies of the future and their families can make the right decisions in the right ways, together with the medical teams caring for them, whatever those decisions may be.
Dr Ravi Jayaram is a consultant paediatrician. This piece was originally posted on Dr Jayaram's Facebook page
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks