NHS doctors turning to substance abuse amid rising levels of stress and burnout
Exclusive: Rising number of GPs seeking help for addiction and mental health problems
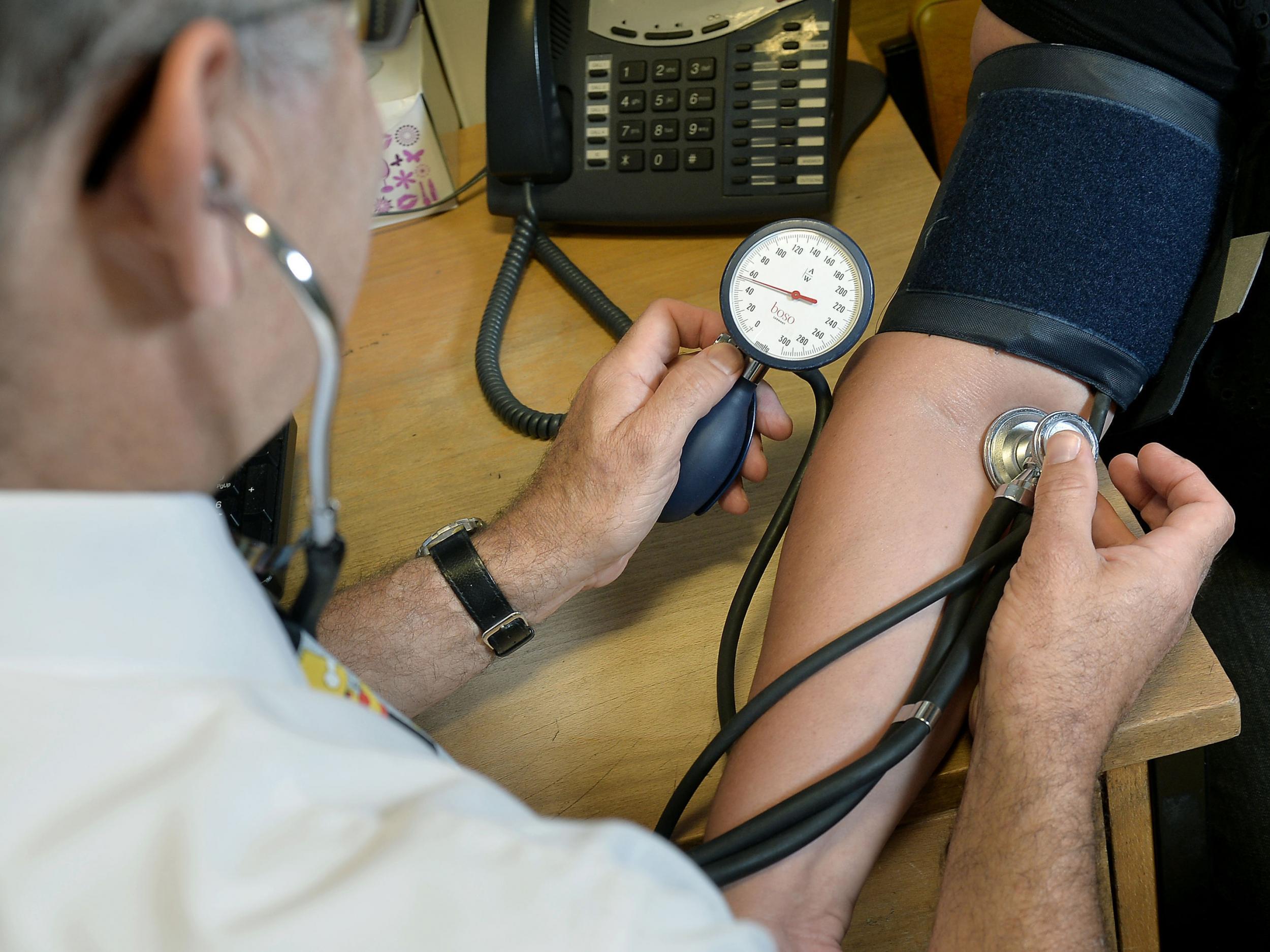
The number of GPs seeking specialist help for substance abuse and mental health problems is “increasing day on day”, the medical director of a new NHS support service for doctors has warned.
Referrals to the GP Health Service have surpassed expectations since its launch in late January, while medics in all fields are seeking help “in escalating numbers”, said Clare Gerada, former chair of the Royal College of GPs. Dr Gerada told The Independent stress and burn-out faced by family doctors with increasingly heavy workloads is contributing to the number of GPs developing severe depression and anxiety, with some turning to alcohol and substance misuse to cope with the pressure.
One GP, currently in recovery, said work-related stress was “definitely” a factor in her rising alcohol intake – which reached the stage where she was calling in sick in the morning because her drinking meant she was not fit to work.
“We are seeing a lot of mental health problems among doctors,” said Dr Gerada. “But I don’t think individual doctors are more or less robust than 10 or 20 years ago.”
“It’s the focus on name and blame, the underfunding, the demands put upon human beings who cannot meet them. It’s the idea constantly told to the public that you can see a GP anytime, anywhere.”
There have been around 400 referrals in the past five months to the to the GP Health Service, which is commissioned to treat around 800 generalist doctors a year, said Dr Gerada.
Doctors around the country are calling for a new government workplace policy and code of conduct to “help prevent and reduce the risk of harm caused by alcohol and substance misuse amongst employees”. The proposals, put forward by members of the British Medical Association (BMA), will be debated at the union’s annual representative meeting next week.
More than half – 52 per cent – of salaried and locum GPs say they have felt unwell due to work-related stress in the last year, according to a BMA survey of more than 2,000 doctors published earlier this month.
The majority of GPs reported an increase in workload, while more than one in 10 said they had taken time off due to stress in the last year. Among salaried GPs, 76 per cent had noted a rise in how much they were required to do.
Sarah*, a GP and recovering alcoholic, told The Independent “the stress levels are enormous” working as a doctor in the NHS.
“Work-related stress was definitely part of it. I'd been a single parent for quite a long time; initially I'd come back from work and just use it to try and relax, and get that feeling of ease,” she said.
“But I was running around, trying to be something for everybody. My alcohol intake gradually went up, until I crossed a line I didn't know I'd crossed, and then couldn't stop.”
She said at first her drinking “wasn't such an issue in the daytime, but later on, I'd have time off sick when I thought I wasn't fit enough to go to work. I'd make up some excuse. I hadn't got to the stage where I was drinking at work, but it was bad enough for me.”
Health Minister Jeremy Hunt has said GP surgeries should be open seven days a week, from 8am to 8pm, and has also announced plans to place doctor generalists in A&E departments to help ease overwhelming pressures faced by NHS hospitals.
However, the number of GPs working full-time has fallen, according to figures published last month, despite Government proposals to recruit 5,000 more by 2020. There are now 34,500 GPs in the NHS, a decrease of 0.3 per cent from last year.
The BMA warned earlier this year that two in every five GPs are planning to quit the NHS amid a crisis of “perilously” low morale.
Sarah said her practice had been “very supportive” and encouraged her to seek help through a non-punitive route, but “even with the most understanding practice in the world, it felt like quite a difficult thing to be honest about – I felt a great deal of shame”.
“I am absolutely convinced there are more GPs in this situation who aren't seeking help,” she said. “A lot of people do drink unhealthily; I'm not saying everyone is at the stage I was at, but I would suspect there's quite a degree of undisclosed alcoholism or drug use, both illegal and prescription pills.”
“Through some of my contacts in recovery, I know some people have looked to prescription drugs to try and manage their symptoms. Certainly things like co-codamol over the counter.”
Sarah said compared to when she first became a GP in the early 1990s, “the demands of work have certainly massively increased. This has taught me I have to look after myself first, otherwise I'm going to kill myself. But that's quite an extreme way to learn that lesson.”
“We’re putting a lot of resources into supporting people because their workloads are too stressful. But why don't we look at the workload,” she said. “There's something particular about dealing with other mental health issues. The work is draining; it's wonderful, but I'm exhausted after a full day's work.
“It's not just the patient contact; it's the huge amount of paperwork we have to do; mandatory training, which we end up doing in our time, because we don't have enough time at work.”
Stephanie de Giorgio, 41, is a locum GP working in East Kent and Deal. She was a partner at a GP practice until last October, but left “because it was making me rather unwell”.
“It was the combination of unlimited demand and fear of making a mistake that was just becoming too great,” she told The Independent. “I was very anxious before going to work in the morning. I'd been unwell with postnatal depression before and that was coming back, so I had to increase my medication. It was the constant feeling like a rabbit in the headlights in work; the fear of making a mistake, which adds to your anxiety.
“Luckily I'm not a drug taker. I may, like many people, have had more gin than is probably healthy – not in a problematic way, but 'gin every night' rather than 'two days a week' because it's something that helps you relax in the evening.”
Dr de Giorgio, who has set up an organisation called Resilient GP to help train and support family doctors and prevent burnout, said pressure on generalists and other doctors has “got massively worse” in recent years.
“There’s a constant pressure to be able to see people when they want it, which is a politically fuelled phenomenon,” she said “We were a practice that prided itself on having very good access times. Our average wait for an appointment with anyone was three days and we'd see anyone who needed to be seen on the day, on the day.
“But that comes at a cost, and that's not leaving at 8 or 9 each night. If you're not managing, you become less efficient, and then the longer you stay at work, and the harder things become.”
Dr Gerada is also medical director of the London-based NHS practitioner health programme, which was set up in 2008 and supports doctors in all specialisms.
“That’s had escalating numbers right across the board, attending for any mental health problem,” she said. “When we started, about 30 per cent were drug and alcohol. But that’s dropped considerably as I think we’ve tapped into unmet need, so now it’s stable at about 7 to 10 per cent.”
NHS England launched the GP Health Service this year “because of particular problems GPs are facing,” she said. “It’s depression, severe anxiety, and some doctors, a smaller number, with alcohol misuse, as an unhealthy coping mechanism.”
Mark Porter, council chair of the BMA, said while medicine is a very rewarding career, “healthcare professionals experience some of the highest rates of workplace stress”.
“It’s concerning that more doctors are feeling stressed by the extreme pressure they’ve been forced to work under as a result of chronic NHS underfunding and staff shortages. Doctors feel demoralised from being stretched so thinly by a government that takes no action on their concerns,” he said.
“The last thing the health service needs is to lose more medical professionals to stress-related illness at a time when hospitals and surgeries are already struggling to cope with rising patient demand and staff vacancies.”
Professor Helen Stokes-Lampard, Chair of the Royal College of GPs, told The Independent “maintaining good mental health for GPs and our team members is imperative for us to deliver the safe care our patients need and deserve.
“But workload in general practice has soared 16 per cent over the last seven years, whilst resources for our service have declined, and our workforce hasn’t risen in step with growing patient demand. We know this has taken its toll amongst our profession, as has been shown by demand for the new NHS GP Health Service.
“The NHS GP Health Service has been one early success of NHS England’s GP Forward View. We now need to ensure it is easily accessible to any GP who needs it, and that it is properly resourced on an ongoing basis to cope with demand.”
A Department of Health spokesperson said: “GPs are the absolute bedrock of the health service which is why this Government has invested £16 million to prioritise their mental health. GPs and trainees can access free, confidential advice if they are experiencing stress, anxiety or other conditions affecting their mental health and wellbeing.”
*Name has been changed
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks