High court dismisses case on ‘failure to give guidance on prioritising patients’
Court was told doctors regularly faced with ‘desperately difficult decisions’ about which patients should first in line for treatment
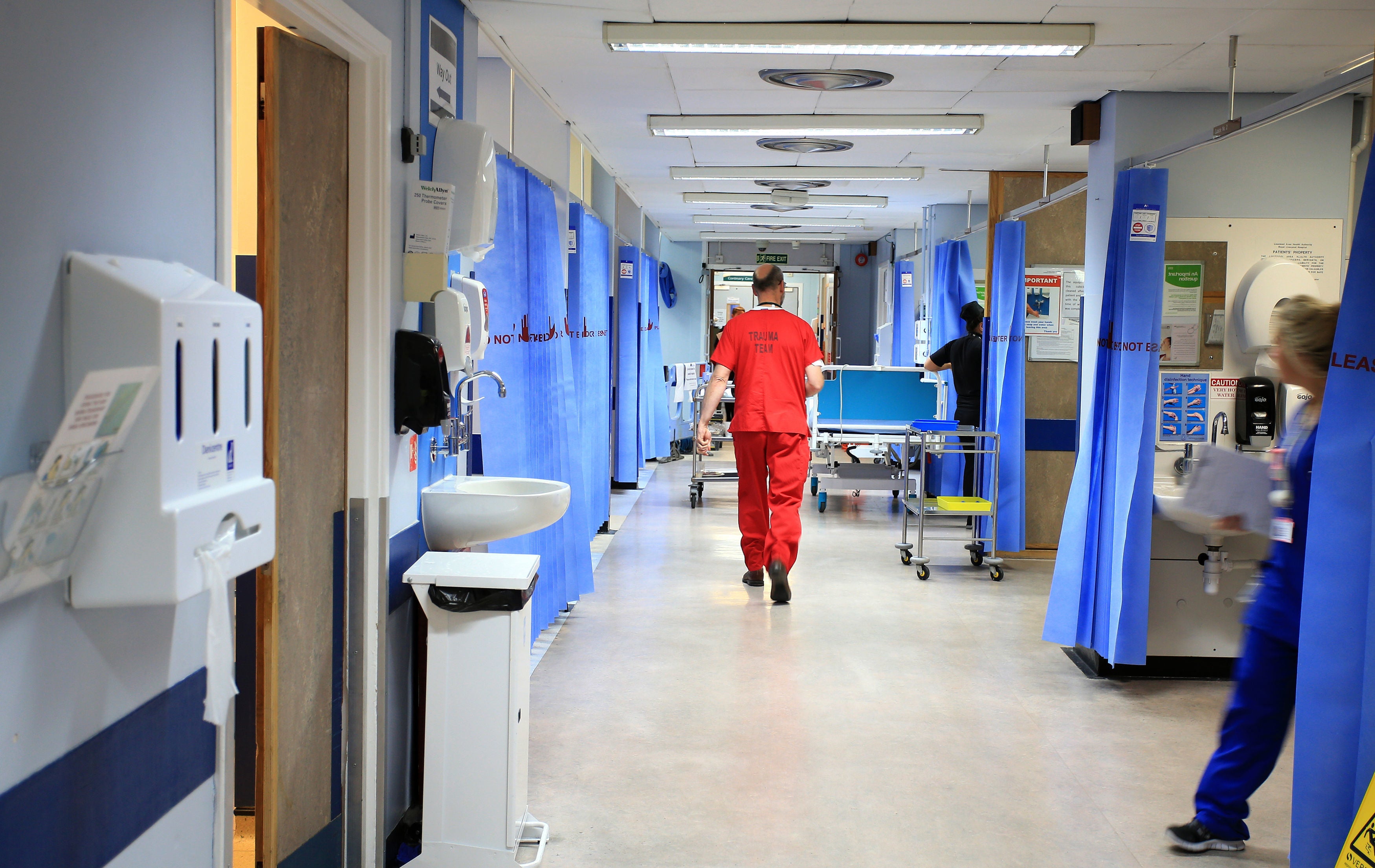
A legal challenge to the government’s alleged failure to issue national guidance on how to prioritise patients during the Covid-19 pandemic has been dismissed by the High Court.
Heather Thomson, a woman from Suffolk in her early 40s with dementia and other “complex health needs,” claimed the Department of Health and Social Care (DHSC) and NHS England’s failure to produce a “national prioritisation policy” could result in “a postcode lottery for patients”.
Her lawyers argued that, without such a policy, there was “a real risk that decisions regarding access to critical care resources will be systematically taken on an inconsistent and arbitrary basis”.
Ms Thomson’s mother Vicky Thomson, who also has underlying health conditions and is “clinically vulnerable to coronavirus”, said that “without the clear national policy, she would only take [her daughter] to hospital as an absolute last resort”.
At a hearing this week, their barrister Vikram Sachdeva QC said: “If it is the case that they are not prioritised for critical care treatment, then the claimants would wish to know as much in advance, so that they can make informed decisions about whether to choose to be treated palliatively in the community, or take the risk of seeking admission to a hospital where they may not be prioritised for access to critical care in any event.”
He told the court that doctors were now regularly faced with “desperately difficult decisions” about which patients should be prioritised for treatment during the coronavirus pandemic, when “finite” resources could be “overwhelmed”.
He said that a decision made in those circumstances on who would get a bed in an intensive treatment unit (ITU) was “not simply a clinical decision, it is a rationing decision”.
But, Mr Sachdeva said, there was still “no policy at all” to give guidance on “how doctors should deal with the terrible question of which patient should get the bed”.
He argued that, without a national policy, decisions about who gets critical care treatment “are being taken pre-emptively by clinicians in both primary and secondary care and by patients”.
Mr Sachdeva said in written submissions: “Patients and their families have the right to understand why, when and how prioritisation decisions will be taken, and that requires nationally developed criteria clearly communicated to members of the public.”
He added: “To leave these decisions to the local or individual level is not just extremely unfair and manifestly unjust to the medical profession, who are working under extreme pressure due to understandably limited resources and at risk of severe moral distress, and patients and their families who do not understand why or how these decisions are being made.
“It also fails the wider public which is entitled to open communication regarding how these decisions are being made.”
He added that publishing such a policy meant that decisions about who received intensive care treatment would be “transparent, so that patients can take an informed decision whether to go to hospital in circumstances in which they may not qualify for an ITU bed”.
Lawyers representing the DHSC and NHS England both said that the claimants’ case was “simply unarguable”.
Refusing permission for the claim to be considered at a full hearing, Mr Justice Swift ruled that neither the DHSC or NHS England were obliged to give guidance on “how resources should be allocated from case to case at the clinical level”.
The judge also said: “It is not even arguably irrational for the Secretary of State not to have the sort of policy the claimants contend for.”
It is understood that the Thomsons are considering whether to bring an appeal against the decision to refuse permission for a full High Court challenge.
Article courtesy of PA
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments



Bookmark popover
Removed from bookmarks